Description of Posterolateral Knee Injuries
Located on the outside of the knee joint, the posterolateral corner (PLC) of the knee functions to stabilize the knee against direct lateral or external forces. Injuries that occur to this area are often due to a sports impact injury – from sports like – football, soccer skiing and basketball. Although injuries to this area of the knee represent a smaller percentage of cases compared to the anterior cruciate ligament (ACL) or medial collateral ligament (MCL), this injury pattern can create a devastating impact on athletic performance.
The posterolateral corner of the knee is one of the more complex areas to both diagnose and surgically treat when injured.
Symptoms of a PLC injury include:
- Side-to-side instability
- Difficulty twisting, turning and pivoting
- Minimal swelling and pain along the outside of the knee
- A foot drop with a concurrent peroneal nerve injury
Patients gradually note the onset of instability patterns over the ensuing weeks to months after injury. This is problematic because the majority of patients are recommended to undergo surgery within the few 2 to 3 weeks after the initial injury to maximize the chance of a successful outcome.
The main anatomic structures of the posterolateral aspect of the knee are the lateral (fibular) collateral ligament (LCL), the popliteus tendon and the popliteofibular ligament. In addition, the lateral capsule, with its thickening called the anterolateral ligament, and the biceps femoris attachment to the fibular head serve as very important stabilizer. Concurrent with these ligaments, it is very important to assess the function of the common peroneal nerve because the nerve crosses the fibular head very close to these structures. Approximately 15-20% of patients may have a common peroneal nerve injury with ankle numbness or weakness who present with a posterolateral corner injury.
Diagnosis of Posterolateral Knee Injuries
There are many tests that must be synthesized to diagnose a posterolateral corner knee injury. These include:
- Varus Stress Test – in full extension and at 30° of knee flexion
- Dial Test at 30° and 90° of knee flexion
- Posterolateral Drawer Test
- External Rotation Recurvatum Test,
- Reverse Pivot Shift Test
- Assessment for a Varus Thrust Gait
All of these tests must be assessed in patients to determine the type of instability present. About 72% of patients who have a PLC injury will also have a concurrent cruciate ligament injury. Thus, one must not overlook the possibility of a posterolateral injury by focusing only on the injured cruciate ligament, because missing a posterolateral knee injury can cause failure of a reconstructed cruciate ligament.
Dr. LaPrade will examine the patient and use plain x-rays, stress x-rays, and often times, an MRI to utilize and examine the injury and to determine whether or not a posterolateral corner injury exists. In many cases, a fracture of the medial tibial plateau and the fibular head will also be present. Posterior kneeling stress x-rays should also be obtained when there is a concern for concurrent PCL tears to determine the amount of any increase in posterior translation on the injured knee.
Posterolateral knee injuries are classified according to the degree of injury:
- Grade I Injury: small partial tear with minimal instability
- Grade II Injury: partial tear with an endpoint to stressing
- Grade III Injury: complete tear with no good endpoint to stressing
In general, all grade III injuries are recommended for surgery because of the low likelihood of healing. This is primarily due to the unique anatomy of the posterolateral corner – there are two opposing convex bony surfaces present which leads to inherent bony instability. In general, due to the high risk of scaring and retraction of torn structures for injuries of the posterolateral knee, it is recommended that most surgeries be performed within two to three weeks after the injury to allow for early range of motion and to make sure sutures can easily be held into the torn structures with early motion after surgery.
Have you sustained a posterolateral knee injury?
There are two ways to initiate a consultation with Dr. LaPrade:
You can provide current X-rays and/or MRIs for a clinical case review with Dr. LaPrade.
You can schedule an office consultation with Dr. LaPrade.
(Please keep reading below for more information on this condition.)
How to Read a MRI of a PLC Injury
Surgical Treatment of PLC Injuries
Dr. LaPrade usually recommends a hybrid approach for repairable structures and an anatomic reconstruction of midsubstance tears of the posterolateral corner in acute injuries; while in chronic injuries he will generally perform anatomic reconstructions.
Dr. LaPrade has developed multiple anatomic-based and biomechanically-validated surgical techniques to treat these injuries to include lateral (fibular) collateral ligament reconstructions, popliteus tendon reconstructions, proximal tibiofibular joint reconstructions, and complete posterolateral corner reconstructions. All of these procedures have been proven to result in positive patient outcomes.
Post-Operative Care for PLC Injuries
The postoperative rehabilitation for these injuries includes allowing motion of 0-90 degrees for the first two weeks within the “safe zone” decided by Dr. LaPrade as he moves the knee and assesses the stress on the repaired structures at the time of surgery and then increasing motion to full after the first two weeks after surgery. Patients are nonweight bearing for six weeks postoperatively and to avoid isolated active hamstring exercises for the first four months postoperatively to avoid significant stress to the healing posterolateral corner repair and reconstruction procedures.
Related Studies
- Outcomes and Surgical Technique of Acute grade III Isolated and Combine PLC Injuries
- Outcomes of an Anatomic Posterolateral Knee Reconstruction
- Varus Stress Radiographs
- Assessment of Healing of Grade III Posterolateral Corner Injuries
- MRI Appearance of the PLC with Surgical Verification
- Analysis of the Static Function of the Popliteus Tendon and Evaluation of an Anatomic Reconstruction
- Mechanical Properties of the Posterolateral Structures of the Knee
- Anatomy and Biomechanics of the Lateral Side of the Knee
- Anatomic Posterolateral Reconstruction – Development of Surgical Technique
- Posterolateral Attachments of the Knee – a Qualitative and Quantitative Analysis
- Effect of Tibial Postioning on the Diagnosis of PLC Rotatory Instability in the PCL Deficent Knee
Posterolateral Corner of the Knee FAQ
1. What is the Posterolateral Corner of the Knee?
The posterolateral corner of the knee involves the structures on the lateral (outside) and posterolateral (outside and back) aspects of the knee. For many years, it was noted to be a very complex area to both diagnose and treat and was often called the “dark side” of the knee due to this. In fact, over two decades ago, many of the surgical procedures to treat the posterolateral corner of the knee were unsuccessful and many patients that sustained this injury had a high risk of having long-term disabling symptoms.
Our research team has performed a very comprehensive series of detailed studies on the anatomy, biomechanics, objective diagnosis, anatomic based biomechanical studies and ultimately clinical outcome studies on the posterolateral corner of the knee. We have published close to 50 peer-reviewed articles on this topic, and have led a comprehensive overhaul of the treatment of this pathology. This has led to new anatomic based reconstruction procedures which have proven to be very successful. In fact, some of our most successful surgeries are those involving the posterolateral corner of the knee because of the very comprehensive analysis that we performed in analyzing these injuries.
2. What are the Main Anatomic Structures of the Posterolateral Corner of the Knee?
There are three main static stabilizers of the posterolateral corner of the knee. These involve the fibular (lateral) collateral ligament, the popliteofibular ligament, and the popliteus tendon. The fibular collateral ligament provides the most stability to preventing side-to-side gapping, whereas the popliteus tendon and popliteofibular ligament are important stabilizers for posterolateral and external rotation of the knee.
There are also many other important structures that are important for providing stability of the posterolateral corner of the knee, including the lateral capsule, the lateral meniscus, the iliotibial band, and the short and long heads of the biceps femoris. Altogether, injuries to these structures require a series of reconstructions of the main static stabilizers, as well as repairs of the other torn structures, to provide the best outcomes for patients.
3. What are the Important Clinical Tests for a Posterolateral Corner Knee Injury?
The most important clinic tests for a posterolateral corner knee injury are the varus stress test in both full knee extension and 30 degrees of knee flexion, the dial test at 30 and 90 degrees, the posterolateral drawer test, and increases in heel height and/or the external rotation recurvatum test. In addition, it is important to have the patient walk to determine if they have a varus-thrust gait.
The varus stress test is performed with the leg over the side of the bed and the examiner holding on to the foot and ankle and pushing it towards the bed to determine if there is any gapping of the lateral compartment. The examiner should have one’s fingers over the joint line to assess for this.
The dial test is performed by holding the knee at 30 and/or 90 degrees in either the supine (lying down) or prone (lying on one’s stomach) position. This is a nonspecific test because it can also be positive in patients that have a medial sided knee injury. This test assesses for the differences in external rotation on the injury compared to the normal knee.
The posterolateral joint test is performed with the knee flexed to 90 degrees and involves rotating the foot to the outside, or externally. With this test, one can see if there is any increasing posterolateral rotation compared to the contralateral knee. This test is important to determine the stabilizing function and congruity of the popliteus tendon. A dynamic assessment of the posterolateral drawer test is called the reverse pivot shift test. This test is relatively nonspecific but involves flexing the knee to 90 degrees, externally rotating the foot, and then straightening the knee to see if the knee “clunks” or slides back into position. Unfortunately, this is a rather nonspecific test because 35% of normal uninjured knees have a positive reverse pivot shift test.
The final important test is to look at the difference in heel heights on the injured compared to the contralateral side. This should be measured in centimeters and helps to provide an assessment of whether there is a combined ACL and posterolateral corner injury. We have found that an increase in heel height of 3 cm in an ACL injured knee is very highly specific for a concurrent fibular collateral ligament tear. The external rotation recurvatum test is a variant of this whereby the knee is so injured that it also slips into external rotation as the femur falls back posteriorly. We also have found that this test is positive in patients with ACL and posterolateral corner injuries. Finally, the varus-thrust gait analysis determines if when the patient is walking if the knee wobbles side-to-side because of gapping at foot strike on the lateral compartment (due to injury to the posterolateral knee structures). This test is also relatively nonspecific because patients who have medial compartment arthritis will also have a varus-thrust gait.
4. What is the Arcuate Ligament?
The arcuate ligament was an old term described to report on the structures which course from the back part of the fibula to the popliteus tendon and posterolateral capsule area. In the early 1900s, it was called the popliteofibular ligament, but this term became lost from literature for many years. Because these structures had a curved, or arcuate shape, they were called the arcuate ligament for many years. More recently, we have recognized the old literature and note that the arcuate ligament is really a combination of specific anatomic structures including the popliteofibular ligament, the capsular arm of the short head of the biceps femoris, and the fabellofibular ligament. Together, these structures help to provide external rotation stability as well as preventing hyperextension of the knee. Thus, the arcuate ligament is an old term that really does not have any specific use in the current literature.
5. How does a Posterolateral Corner Injury happen?
We have found that most posterolateral corner injuries occur due to a hyperextension injury, a contact hyperextension injury, or an injury which causes the outside of the knee to open up due to stress on the knee, which can often include a blow on the inside (medial) part of the knee. With multiple ligament injuries, sometimes it can be very difficult to determine what the cause of the injury was, and in motor vehicle accidents it is often difficult to determine the etiology of the posterolateral corner injury. It is important to recognize with posterolateral corner injuries that the common peroneal nerve can be involved in up to 15% of patients so any sensory or motor deficits for this nerve should always be checked for.
6. What are the Main Structures to look for on MRI Scans of Posterolateral Corner Injuries?
The main structures to look for on MRI scans of the posterolateral corner of the knee are the fibular collateral ligament, the popliteus tendon, and the popliteofibular ligament as well as the biceps femoris attachments to the fibular head, the lateral capsule, and the iliotibial band.
We have validated with our research studies that injuries to the fibular collateral ligament, especially in chronic cases, are very difficult to diagnosis on MRI scans. In fact, only about 70% of the time an MRI can be accurate for injuries to the fibular collateral ligament. Thus, when there is some concern that the patient has increases in gapping and it appears that the FCL is intact, it may in actually be stretched out and nonfunctional and bilateral varus stress x-rays should be obtained to objectively diagnose this pathology.
Looking at the popliteus tendon involves assessment of its attachment site on the femur as well as its musculotendinous junction. These injuries are best determined acutely, because on chronic injuries the popliteus tendon can be stretched out and nonfunctional and they can look intact on an MRI scan.
The popliteofibular ligament is a very thin structure, so it is important to ensure that the MRI cuts pass through it before determining if there is an injury to either knot.
Assessment of the lateral capsule is important because when the lateral capsule is completely torn off the tibia, it can make the knee severely unstable.
Injuries to the biceps femoris attachment to the fibular head are particularly important because these injuries often are associated with injuries to the common peroneal nerve. In addition, even if the common peroneal nerve is intact or minimally injured, it can be malpositioned when there is an avulsion fracture (called an “arcuate fracture”) of the biceps femoris off the fibular head. This is very important to assess for prior to a surgical reconstruction to ensure that one is very careful in approaching the posterolateral corner of the knee because when the biceps femoris is avulsed because of the common peroneal nerve may be malpositioned with this injury pattern.
Finally, the iliotibial band attachment site at Gerdy’s tubercle on the tibia is also important to assess for. We have found the iliotibial band to be injured in only 3% of posterolateral corner injuries, so when this is injured, it is usually with a very severe posterolateral corner injury present.
7. What X-rays are Important to Assess for Posterolateral Corner Injuries?
In the acute situation, it is important to obtain standard anterior to posterior (front to back), a standing Rosenberg view, and lateral x-rays to assess for any possible medial compartment fractures due to the increasing gapping laterally causing pressure in the medial compartment. One can also look for an avulsion of the fibular head (an “arcuate fracture”), which can indicate that the main structures which attach here (the biceps femoris, fabellofibular ligament, popliteofibular ligament, and biceps femoris tendon) may be avulsed off with this injury pattern. In addition, looking for a small avulsion fracture of the lateral capsule, called a Segond fracture, should also be assessed for.
For chronic injuries, it is important to obtain these prior x-rays as well as to obtain a standing Rosenberg view to assess for medial compartment joint space narrowing as well as a long leg alignment x-ray. It is very important to obtain a long leg alignment x-ray in chronic posterolateral corner injuries because it has been reported that repairs or reconstructions in patients who have a varus alignment have a very high risk of having a posterolateral corner reconstruction stretch out due to the extra stresses placed here. Thus, these patients often need a first stage proximal tibial osteotomy prior to a complete posterolateral corner reconstruction to prevent the reconstruction grafts from stretching out.
Perhaps the most important x-rays to obtain in documenting objectively a posterolateral corner injury, which are definitely better than most physical examinations, are bilateral varus stress x-rays. We have found that increases of lateral compartment gapping of between 2.4 to 2.7 mm are consistent with a complete tear (or a stretched and nonfunctional FCL) of the fibular collateral ligament when compared to the contralateral side. In addition, increases of varus gapping of 4.0 mm or more are consistent with a complete posterolateral corner injury. In addition, because of the high risk of a combined PCL and posterolateral corner injury, obtaining bilateral PCL stress x-rays is also an important assessment to determine if there is a combined PCL and posterolateral corner injury. An isolated PCL injury usually has between 8 to 12 mm of increased posterior tibial translation compared to the contralateral side, while 12 mm or more of increased posterior tibial translation usually demonstrates a combined PCL and often have combined a posterolateral corner injury to result in this much increase in posterior tibial translation.
8. What is the Cause of Posterolateral Nerve Pain?
The main cause of posterolateral corner nerve pain is compression or irritation of the common peroneal nerve. The common peroneal nerve provides sensation on the lateral aspect of the leg and the top of the foot. Injuries to the common peroneal nerve from a posterolateral corner injury, a multi-ligament knee injury, or direct trauma can result in pain along the posterolateral corner of the knee, especially in the region of the fibular head and styloid. It is important to assess if an injury has caused these pathologies because patients may also have pain and irritation at this area of the knee when they may have a herniated disc or compression of a nerve in the low lumbar spine area.
Thus, a thorough evaluation of both the knee and also an evaluation of the cause of any associated back pain for a potential for disc pathology needs to be assessed concurrently in the patients. When there is localized compression of the common peroneal nerve, one needs to assess if it is due to a combined posterolateral corner injury, a proximal tibiofibular joint injury or instability, or if it is localized compression. This can make the difference in terms of the recommended treatment, which can include a complete posterolateral corner reconstruction, a fibular collateral ligament reconstruction, a proximal tibiofibular joint ligament reconstruction, or possibly a localized common peroneal nerve neurolysis if there is no other pathology identified in this area of the knee which localizes to causing the peroneal nerve symptoms.
9. What is the Main Surgical Approach to the Posterolateral Corner of the Knee?
We have developed a surgical approach which is used by most surgeons to approach the posterolateral corner of the knee. The incision extends from the inferior portion of the iliotibial band down over close to Gerdy’s tubercle and then over the anterior compartment of the leg. Dissection is then carried down to the superficial layer of the iliotibial band and over the long and short heads of the biceps femoris. A common peroneal nerve neurolysis was then performed. This allows for a wide view of the main structures of the posterolateral corner of the knee.
Incisions to approach the fibular collateral ligament attachment on the lateral aspect of the fibular head involve making an incision into the biceps bursa close to the fibular head and then dissecting the remnants of the FCL off the lateral aspect of the fibular head.
Approaches to the fibular collateral ligament and popliteus tendon attachment on the femur involve making an incision through the iliotibial band and then a small incision in the lateral capsule to identify the popliteus tendon attachment on the femur and then measuring 18.5 mm (on average) posterior to this to identify where the fibular collateral ligament attachment site is located on the femur. These anatomic measurements are very important for severe or chronic posterolateral corner injuries because the native anatomy may not be present and anatomic-based reconstructions are critical to providing the best surgical outcomes for these patients.
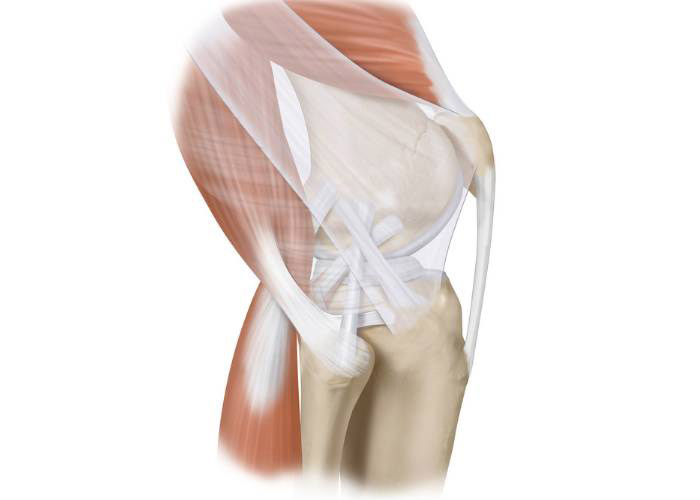
10. What is involved with a Reconstruction of the Fibular (lateral) Collateral Ligament?
The fibular collateral ligament is the most important stabilizer of the knee to preventing the knee from gapping side-to-side due to lateral compartment opening. It attaches in a sulcus on the femur, on average 18.5 mm posterior from the popliteus tendon attachment on the femur, and it courses down to attach to the lateral aspect of the fibular head. It is located approximately 40% back from the anterior margin of the fibular head when one measures from anterior to posterior. Its average length is approximately 70 mm. Thus, it is important to recognize these attachment sites as well as total length of the ligament in choosing a reconstruction graft.
We have developed an anatomic base reconstruction and have published several very successful outcome studies on the fibular collateral ligament reconstruction technique. It involves harvesting a hamstring graft, or using a hamstring allograft, and then placing reconstruction tunnels at the two attachment sites of the fibular collateral ligament and then passing the graft into these tunnels and fixing it in place with interference screws. We have found this technique to be one of our most successful surgeries, with outcomes similar to ACL reconstructions.
It is important to recognize that other grafts may be viable for this technique, but the diameter and strength of the hamstring grafts has proven to result in very successful surgery. It is also important to recognize that the patellar tendon graft is not a good graft for this particular reconstruction because it is too short to be able to ensure an anatomic reconstruction of the fibular collateral ligament.
11. What is involved with a Complete Posterolateral Corner Reconstruction?
A complete posterolateral corner reconstruction is performed when there is a complete tear of the fibular collateral ligament, popliteus tendon, and popliteofibular ligament and the knee is very unstable. We have developed and successfully validated an internationally utilized anatomic-based reconstruction for this injury pattern twenty years ago, and prior to this, most reconstruction techniques involved slings or repair procedures that were at risk for failure, with most of them having almost a 40% failure rate.
We were able to perform very detailed quantitative anatomy studies and then biomechanical studies, following it with anatomic-based reconstruction procedures in the lab and have validated with clinical studies that these surgeries are very successful. They involve reconstructing the three main static stabilizers of the posterolateral corner of the knee which include the popliteus tendon, the popliteofibular ligament, and the fibular collateral ligament. We do this by placing four separate reconstruction graft tunnels at the posterolateral corner of the knee with two in the femur for the attachment sites of the popliteus tendon and fibular collateral ligament, one in the fibular head for the attachment site of the fibular collateral ligament and then a tunnel in the tibia where by the popliteus tendon and popliteofibular ligament grafts are placed to provide static stability to the knee for these structures. We have had long-term follow-up on these patients and note that these grafts are very successful at restoring stability to the knee with these patients with these complex procedures.
12. What does one look for in an Injury to Posterolateral Structures during an Arthroscopy?
We have published on the arthroscopic appearance of posterolateral corner knee injuries. First, because of the increase in lateral compartment gapping (varus opening) of the posterolateral corner of the knee with these injuries, we have described a “drive-thru” sign that is seen with this injury pattern. In most instances, it can be somewhat tight and more difficult to see things in the posterolateral corner of the knee when an arthroscope is used, especially in normal knees. In the knee with a posterolateral corner injury, there can be a significant amount of gapping whereby it is very easy to see all of the structures in the posterolateral corner of the knee. This is what we call a “drive-thru” sign. In addition, we can assess the entire aspect of the lateral meniscus from its root attachment all the way along the popliteal hiatus and anteriorly to assess the structure and function and determine if there is any injury to the lateral meniscus when there is a drive-thru sign.
Viewing along the lateral gutter, the integrity of the popliteus tendon on its femoral attachment site is able to be performed as well as an assessment of the popliteofibular ligament and popliteomeniscal ligaments attachments to the lateral meniscus. It is not possible to judge an injury of the popliteus musculotendinous junction, but one can have a secondary sign assessment of this by using a probe and pulling on the popliteus tendon to determine if it is loose below the meniscus at this location. In addition, it can get difficult to arthroscopically visualize if the lateral capsule was avulsed with these injuries, but one can see that the lateral meniscus will pull away from the tibia when one is applying a varus stress to the knee during an arthroscopic examination to validate that the lateral capsule is torn off the tibia. This assessment can also be performed when there is a Segond fracture with an ACL tear to determine if the lateral meniscus is potentially unstable with this injury pattern.
13. What is involved with Posterolateral Knee Rehabilitation?
There have been many advancements in the treatment of postoperative rehabilitation principals for the posterolateral corner of the knee. In particular, have validated that early range of motion does not cause the grafts to stretch out and improves patient function. In addition, early motion has been validated to minimize the risk of postoperative stiffness (arthrofibrosis).
Twenty years ago, most posterolateral corner knee injuries were treated with cast and with knee flexion to try to get the tissues to scar back in so that they would not stretch out. We have found that with our anatomic base reconstructions that one can start early motion to improve patient function and minimize the risk of stiffness. Our two year minimum follow-up stress x-rays have documented that there is no stretching out at all of these grafts and that this is a safe and effective procedure.
In addition, presently, these patients are kept non-weight bearing. This is felt because these injuries are very severe and the body needs time to ensure that the grafts heal.
We have found that because of our excellent success with reconstructions of the fibular collateral ligament, a prospective study evaluating the differences between partial 40% weight bearing and non-weight bearing of the fibular collateral ligament were successful in validating that early partial weight bearing of FCL reconstructions both did not cause the FCL graft to stretch out and actually the patients had improved early function postoperatively.
Thus, our current postoperative rehabilitation protocol for isolated reconstructions of the fibular collateral ligament and also for those combined concurrent with an ACL reconstruction (where most ACL reconstructions nowadays are fully weight bearing postoperatively) have the patient partial weight bearing and this has greatly improved function their function.
We are currently moving forward with studies to evaluate partial weight bearing versus complete weight bearing for fibular collateral ligament reconstructions and non-weight bearing versus partial weight bearing for complete posterolateral corner reconstructions using level 1 evidence to validate that further advancement of our rehabilitation protocols is possible because of our early work at developing solid anatomic-based posterolateral corner reconstruction procedures.
14. What Bone Bruises are seen with Posterolateral Corner Injuries?
Since a posterolateral corner injury involves gapping and extra stress on the outside of the knee, it can often cause compression towards the inside of the knee. In up to 10% of patients, this may result in a fracture of the medial tibial plateau. In addition, it often involves bruising of the bone, called a bone bruise, on either the medial femoral condyle or medial tibial plateau or both, on the inside of the knee. When one does see bone bruising of the medial compartment, one has to be concerned that it is a secondary sign of posterolateral corner injury and the patient should be very carefully assessed to rule out a concurrent FCL or posterolateral corner knee injury in this circumstance.
15. What is a Fabella on the Posterolateral Corner of the Knee?
The fabella is a sesamoid bone that is located within the lateral gastrocnemius tendon in the posterolateral corner of the knee. Radiographic studies have shown that it is present in 38% of human knees.
This piece of bone forms where the lateral gastrocnemius tendon merges with the posterolateral capsule of the knee. Thus, the bone is intraarticular and does have a small area of articular cartilage over it. In some circumstances, patients may develop arthritis of this portion of the joint and the arthritic fabella may cause wear and a grooving of the cartilage on the lateral femoral condyle. These patients often have pain that is well localized to this area of the knee. The patients with an irritated fabella, called “fabella syndrome”, may benefit from an arthroscopic assisted excision of this piece of bone to decrease pain in this area. We have found that this surgery to be successful in the vast majority of patients at relieving pain in this region of the knee.
16. When can Posterolateral Corner Knee Injuries be Repaired?
The posterolateral corner of the knee is very unique and that there is a lack of bony stability to this area of the knee. This is because there are two convex opposing surfaces of the lateral femoral condyle and lateral tibial plateau. Thus, human and animal studies have documented that these injuries usually do not heal. This is different than the medial side of the knee where there is bony stability and most MCL injures will heal when they are isolated.
Because of this inherent bony instability, extra stress is placed on any repaired knee structures. There have been studies that have shown that the success rates with repairs are approximately 60% on the posterolateral corner of the knee, whereas the success rates of reconstructions are 90% or higher. Because of this, we have recommended that reconstructions be performed in almost all circumstances instead of repairs. I tell my patients that when I went to college I wanted to get As rather Ds and that is the difference in the posterolateral knee reconstruction versus repair outcomes in these areas. Unfortunately, there are still some surgeons today who recommend repairs because they feel that a surgical approach to the posterolateral corner of the knee can be quite challenging, and we would recommend that they consider reconstructions instead of repairs for the vast majority of these tears to maximize patient outcomes. When one knows the anatomy, these reconstructions are quite simple and give the best chance of having the best patient outcomes over time.
17. What is a Good Summary about Posterolateral Corner Injuries of the Knee?
A good summary for the posterolateral corner of the knee is that one should assess the anatomy and determine the injury pattern. Obtaining an objective diagnosis with varus stress x-rays can confirm that a complete posterolateral corner or fibular collateral ligament injury is present. Because of the low chance of healing with nonoperative treatment, bracing or casting is not recommended. Patients do best if they have surgery acutely instead of chronically in the posterolateral corner of the knee, especially if they have an underlying varus alignment (bow leggedness) to their knee.
Anatomic-based reconstructions, which we have developed in my research lab, have proven in clinical studies to be very successful at restoring patients back to activities. In addition, modern rehabilitation techniques with early motion and progressive strengthening have also validated that patients can be restored back to high levels of activity in these patients. Thus, while in the past many patients did poorly and it was called the “dark side” of the knee, we have performed a very comprehensive body of research studies which have significantly improved the overall diagnosis, treatment and ultimately patient outcomes with these very complex injuries. Thus, the posterolateral corner of the knee can now be certainly celebrated as no longer being the “dark side” of the knee!
