Description of Medial Meniscus Tear
The medial meniscus is an important shock absorber on the inside (medial) aspect of the knee joint. It absorbs about 50% of the shock of the medial compartment. Thus, when there is a medial knee injury such as a medial meniscus tear, it is very important to try to repair the tear, because if not repaired and is trimmed out there will be an increase to the load on the medial compartment, which ultimately leads to osteoarthritis.
A medial meniscus tear is more common than a lateral meniscus tear, because it is firmly attached to the deep medial collateral ligament and the joint capsule. In addition, the medial meniscus absorbs up to 50% of the shock of the medial compartment, making the medial meniscus susceptible to injury.
Medial meniscus tears appear in a variety of patterns:
- Longitudinal
- Bucket-handle
- Displaced bucket handle
- Root detachments
- Parrot beak
- Radial
- Displaced flap
- Horizontal
- Degenerative
Symptoms of a medial meniscus tear:
- Pain
- Swelling and stiffness, increases gradually over 2 to 3 days
- Catching or locking
- Instability
A complex tear of the medial meniscus includes a combination of any of the patterns listed above. In many circumstances in patients with these tears, the meniscus needs to be trimmed out. However, this does increase the risk of osteoarthritis, especially in patients who continue to participate in impact activities.
MRI Diagnostic
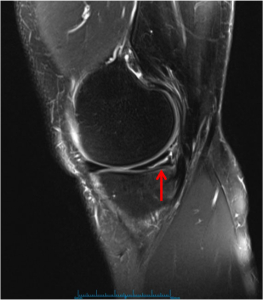
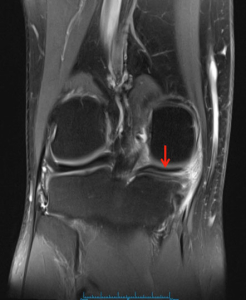
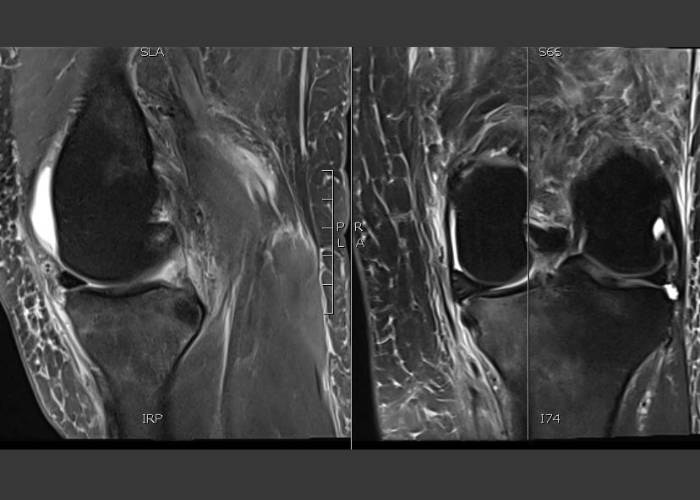
How to Read an MRI of a Medial Meniscus Tear
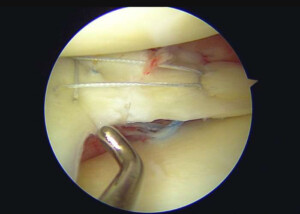
How is a medial meniscus tear repaired?
Research has justified that patients with a certain age, with a proper environment, fairly normal articular cartilage, and neutral or near normal alignment, should have an attempt at a repair for medial meniscus tears. We believe that trying to stimulate an improved healing environment through the use of bone marrow elements, platelet rich plasma (PRP), and a large number inside-out meniscal repair sutures, can lead to improved ability to heal these tears, especially in younger patients.
How long for medial meniscus tear to heal?
The treatment for patients who undergo a partial medial meniscectomy is to initiate physical therapy on the first day after surgery. A treatment regimen working on reactivation of the quadriceps muscles, regaining of full knee and patellar mobility, and a quick resolution of knee swelling is emphasized. In general, we recommend that patients who have a minimal amount of meniscus trimmed out hold back on any impact activities until a minimum of 6 weeks after surgery. In patients who have a significant amount of meniscus resected, it is often recommended to avoid significant impact activities due to the higher risk of the development of osteoarthritis in these patients with this activity.
When a medial knee injury such as a torn medial meniscus needs to be resected, we strongly recommend that these patients be followed very closely. Patients need to report back to their physician if they have any pain or swelling with activities, because these are the signs of arthritis and may indicate further progression of arthritic changes. If this is present, further treatment to include activity modification, low impact exercising, unloader braces, injections, or possible meniscal transplantation may be indicated.
It is almost inevitable that when one has a significant amount of the medial meniscus resected that they will develop further arthritic changes over time. Because not everybody is the same, these changes can develop within a few weeks up to over a decade. Thus, one of the important things is to recognize that if one has any pain or swelling, they should follow up to make sure they are not developing any joint space narrowing or bone spurs, which would indicate that the medial compartment articular cartilage is wearing out.
Related Studies
- Anatomic Analysis of the Posterior Root Attachments of the Menisci
- Posterior Root Avulsion Fracture of the Medial Meniscus
- Not Your Father’s (or Mother’s) Meniscus Surgery
- Anterior Intermeniscal Ligament of the Knee – An Anatomical Study
- Popliteomeniscal Fascial Tears Causing Symptomatic Lateral Compartment Knee Pain
- Prospective Outcomes Study of Meniscal Allograft Transplantation
Complex Medial Meniscus Tear FAQ
1. What is a complex medial meniscus tear?
Complex medial meniscus tears can mean many things. They can mean that they are large tears, which are reparable, or they can mean that they are very complex or macerated tears that are not reparable. It is important to define the difference between these two in choosing a treatment going forward.
Complex reparable medial meniscal tear can include long tears along the junction of the back of the meniscus and the joint lining (meniscocapsular tears, meniscal root tears, or radial tears). While these tears are felt to be very complex in many circumstances, with the correct surgical team and tools, they can often be repaired.
This contrasts with tears where there is significant maceration, separation, or chronicity of the tear where the chance of a repair is slim to none. In these circumstances, due to the fact the meniscus has a relatively poor blood supply, the only option is to learn to live with the symptoms, and possibly end up with a bigger tear over time, or to consider having a meniscus resection. Unfortunately, meniscus resections almost always lead to the onset or progression of arthritis, so this must be carefully chosen as an option in these circumstances.
2. What does a medial meniscus tear feel like?
Most new onset, or acute, medial meniscus tears do cause pain. The pain is usually located along the inner portion of the joint, at the joint line, or in the back of the knee, especially when one squats down. Tears in the front part of the meniscus are less rare, but these can cause problems going down hills or down stairs. Longstanding meniscus tears, or chronic tears, may or may not cause symptoms. Usually when they do cause symptoms, people will notice them when they have possibly a further tear of an underlying tear, and there will be pain along the joint line with squatting, twisting, turning, or kicking type maneuvers.
3. How does a medial meniscus tear happen?
A medial meniscus tear can happen from many factors. First, a sporting injury can cause it. Medial meniscus tears commonly happen with an ACL tear. This is because the medial meniscus acts as a secondary stabilizer to prevent the knee from slipping forward, and when the ACL tear happens, it puts extra stress on the medial meniscus which leads to it tearing. In addition, deep squats put extra stress on the back of the knee and can cause a medial meniscus tear to occur. Other causes include twisting, turning, or pivoting type activities where extra stress is placed on the inside of the knee, whereby a medial meniscus tear can occur.
4. When does a medial meniscus tear require surgery?
Meniscal tears require surgery both when they are causing symptoms, such as pain with twisting, turning, pivoting, or pain in the back of the knee while squatting, or when there is a complex tear, such as a meniscocapsular tear, a radial tear, or a meniscus root tear, whereby the meniscus is at high risk for further tearing and the development of arthritis if it is not repaired. In these circumstances, if the patient is a good candidate with a relatively younger age and good cartilage surfaces, a meniscus repair would be indicated to address the tear and prevent further progression of osteoarthritis.
5. How do medial meniscus tears occur in athletes?
Most medial meniscus tears that occur in athletes occur due to contact or noncontact twisting mechanisms. A large majority of these occur with a concurrent anterior cruciate ligament tear, where the joint slips forward with an ACL tear commonly results in tears the meniscus away from its attachment at the joint lining. Other types of tears in athletes can occur with significant stresses, or with activities that results in deep-knee flexion, such as a hyperflexion injury while skiing or while playing football. In these circumstances, the extra stress that is placed on the back of the knee can cause either a tear at the lining of the meniscus or it can cause it to be torn away from its bony attachment, which is called a posterior horn medial meniscus root tear.