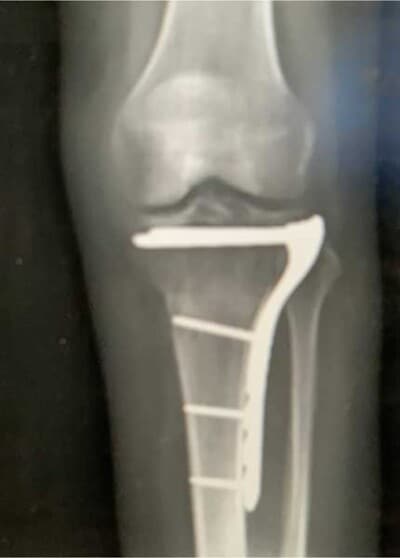
What is a tibial plateau fracture?
Tibial plateau fractures are caused by a force driving the lower end of the femur (thigh bone) into the soft bone of the tibial plateau. The tibial plateau is made of cancellous bone, which is softer than the thicker bone lower in the tibia. An impact often causes the cancellous bone to compress and remain sunken. This damage to the tibial plateau may result in improper limb alignment, and over time can lead to arthritis, instability, and loss of motion in the knee.
The portion of the shin bone (tibia) that is closer to the knee has two relatively flat areas that support the thigh bone (the femur) called:
- Medial tibial plateau (inner)
- Lateral tibial plateau (outer)
They are the main supporting structures for the knee joint. When this portion of the knee becomes fractured, it is called a tibial plateau fracture.
It is not uncommon for athletes such as skiers, basketball players, football players, and court players to sustain a “bruise” of the bone during athletic activity. In these circumstances, the bone sustains enough of a load that there is some swelling of the bone but an actual fracture does not occur. In some of these instances, such as with an ACL tear, there can be a disruption of the bone with a small fracture that only shows up on an MRI scan. These types of fractures have a very good prognosis and a period of time to allow the bone bruise and fracture to heal is required.
How do you diagnose a tibial plateau fracture?
Tibial plateau fractures range from very small fractures that are only seen on MRI scans, to significant injuries that result in a Humpty-Dumpty appearance of several bone pieces nearly impossible to put back together. While those with fractures that only show up on MRI scan have an excellent outcome and a fairly quick return to activities, those involving significant disruption with multiple pieces of the lateral tibial plateau often have a poor prognosis.
What are the symptoms of a tibial plateau fracture?
- Pain when weight is applied
- Swelling
- Limited range of motion
- Severe cases – numbness or “pins and needles” in the foot due to nerve damage
What are the types of tibial plateau fractures?
There are many different types of tibial plateau fractures, and treatment can include both nonoperative and operative programs. To make the best judgement as to whether nonsurgical or surgical treatment should be performed, it’s important to:
- Understand the type of tibial plateau fracture that is present – whether it involves either the medial or lateral plateaus or both
- Assess whether there are other fractures or injuries present
Minimally displaced tibial plateau fractures:
A tibial plateau fracture that is minimally displaced means that the ends of the fracture are displaced less than 1 to 2 mm. There is a good chance that this type of fracture will not displace any further, which we call subside, and it can often be treated without surgery. These types of fractures are often discovered in patients who injure themselves, have x-rays that do not show a fracture and later obtain an MRI scan which shows the fracture. In many circumstances, these patients may have already been walking around or at least putting some weight on their knees for a few days, which would mean that there is a very low chance that this type of fracture would displace further. The general feeling is that these fractures should be treated nonoperatively for up to six weeks to ensure that the fracture heals in a good position and doesn’t become displaced with any further loading to the knee joint itself.
Fractures involving only one tibial plateau:
For tibial plateau fractures that are in a critical location or that have a significant step-off deformity, we recommend surgery to restore the joint surface in almost all circumstances . This is important because when the joint surface is not lined up, there is a much higher risk for the patient to develop traumatic arthritis. There are multiple classification schemes for these types of fractures, but the most common are involving only one of the tibial plateaus (medial or lateral). A thorough assessment of the overall extent of the fracture, the patient’s health history, and any other factors that may concurrently occur with this type of fracture is important in determining who requires surgery and what type of plates and/or screws should be utilized.
Fractures involving both tibial plateaus:
For fractures that involve both tibial plateaus, there is often concern about significant instability and displacement. Even if there is just minimal displacement caused by a fracture involving both tibial plateaus, a surgical fixation may be recommended to give the patient the best chance of having a positive long-term outcome. For those who do have a very severe fracture with multiple pieces – almost like Humpty Dumpty – the goal of surgery may solely be to get the joint surface together as best as possible in anticipation of a potential knee replacement once the fracture fragments heal and the arthritis pain becomes more significant.
What is the treatment for a tibial plateau fracture?
In cases where there is solely a bone bruise or a very mild nondisplaced fracture, the treatment can vary dramatically compared to those where there is a complete fracture or any step-off deformity or comminution of the fracture.
Bone bruise or a nondisplaced fracture:
In cases where there is a bone bruise or a nondisplaced fracture that does not cause significant pain, such as in high-level athletes, a rehabilitation program to allow the swelling to resolve followed quickly by a low-impact exercise program, including low resistance cycling and working in a pool, can help to maintain one’s cardiovascular endurance and allow for a quicker return to activities.
Bone bruise with a small fracture:
In circumstances where there is bone bruise with a small fracture that is not displaced, surgery is not required. If the athlete is able to participate in low-impact activities without having any problems with pain or swelling, they can often maintain their cardiovascular reserves to the point where they do not need an extended period of time after the fracture heals to return to sporting activities.
Tibial plateau fractures requiring surgery:
We have found it very beneficial to concurrently fix tibial plateau fractures with an arthroscope viewing inside the knee to assess the reduction of the joint surfaces during the surgical fixation. This ensures that the fracture pieces are put back together as closely as possible which may not be possible if one is relying solely on x-rays to determine if the fracture is reduced.
How long does it take to recover from a tibial plateau fracture or injury?
A minimum of 6 weeks is usually necessary to allow the fracture to completely heal so that there is no risk of a reinjury. In fractures with a larger disruption of the bone, the athlete may need to be non-weightbearing for 6 weeks and then will need time to recover from the atrophy of not walking on that extremity prior to returning to activities. A slow progression off crutches may then be performed once the athete can walk without a limp and x-rays show sufficient healing. Every plateau fracture is different, so judging the timing of a return to activities is injury specific.
For athletes who require surgery to stabilize the fracture or restore the step-off deformity; the downtime is usually much extended with at least 6 weeks of non-weightbearing and up to several months of rehabilitation to restore overall strength. In cases with significant traumatic arthritis due to cartilage damage, continued problems with pain or swelling may affect the athlete’s ability to return to high-level activities and can affect the length of their athletic career. In circumstances of extreme atrophy, arthritis or multiple fracture, it can take 12 weeks or longer to return to activities.