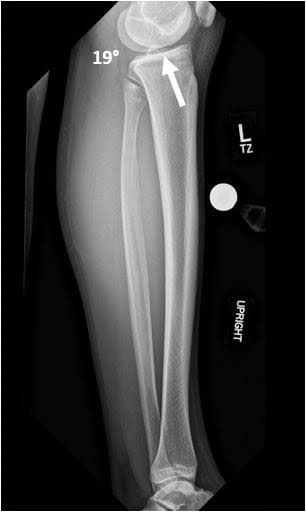
What is a Proximal Tibial Osteotomy?
Proximal tibial osteotomies, equivalent to high tibial osteotomies, involve taking a patient who is bow-legged and making them have either normal alignment through the center of the knee or slightly knock-kneed. This involves creating a surgical fracture on the proximal aspect of the tibia, usually on the inside part, which involves cracking bone of the tibia, leaving a 10-15 mm size hinge of bone intact on the lateral aspect of the tibia, and opening it up to allow the leg alignment to swing over. This is the opening wedge portion of it. A plate and screws are then used to hold it in place and bone graft is inserted into the opening wedge that is created.
Do I Need a Proximal Tibial Osteotomy?
There are 3 main indications for performing proximal or high tibial osteotomies. The most common is in patients who have developed arthritis on the inside of their knee, most commonly due to having a previous partial medial meniscectomy, and who are bow-legged and the rest of the knee cartilage is fairly well intact. In these patients, creating a proximal tibial osteotomy and shifting the weight over to the center or outside of their knee has been found to be very effective in relieving the symptoms of arthritis and to put off needing a partial or total knee replacement. It is generally felt that in younger patients, which are felt to be younger than 50 years old, that a proximal tibial osteotomy is strongly desired over a partial knee replacement because the patient can still participate in high-level activities and high-work activities, without the worry of wearing out the metal and plastic from a partial knee replacement.
The other common indication for performing a proximal tibial osteotomy is in patients that are bow-legged and in need of a medial meniscus transplant, and/or a medial compartment cartilage resurfacing procedure. It is generally felt that the risk of having a meniscus transplant or cartilage resurfacing procedure fail are very high if the patient is bow-legged and the procedure is on the inside part of the knee. Thus, performing a proximal tibial osteotomy either concurrent with or prior to the cartilage resurfacing procedure and meniscal transplant, it would be indicated.
The other most common reason for performing a proximal tibial osteotomy is in patients who have ligament problems. For patients who have a chronic posterolateral corner injury that are bow-legged, the risk of having the graft on the outside of their knee stretch out is very high and it is generally felt that one should have a proximal tibial osteotomy performed either prior to or concurrent with the lateral collateral ligament and posterolateral corner reconstruction. Other indications include patients who have a cruciate ligament reconstruction and who have a tilt of their tibia. Most commonly, a tilt backwards of the tibia with an ACL tear causes an ACL graft to have a high risk of failure and a closing wedge osteotomy would help to unload this. This was already found out by our veterinary colleagues many years ago where they found out that ACL surgeries did not work in dogs because the tibia was tilted so far posterior. Thus, almost all dog “ACL reconstructions” are actually a closing wedge proximal tibial osteotomy, which works quite well in these circumstances. The other indication would be in patients who have a flat tibial slope and who have a PCL tear that is chronic, especially in those who may have some medial compartment arthritis. Increasing the slope in these patients, by tilting the tibia back, is also found to be very effective at providing stability to PCL-deficient knees, and some patients may find that they have enough stability that they do not need a later PCL reconstruction.
Does Bow-Legged Require Surgery?
In patients who have osteoarthritis in the inside part of their knee and who are bow-legged, the use of a medial compartment unloader brace can be an effective screening tool to determine if an osteotomy would be indicated. Thus, we recommend using the medial compartment unloader brace in these patients because we have found them to effectively predict those patients who will do well from a proximal tibial osteotomy.
How Successful is a Proximal Tibial Osteotomy?
The outcomes of proximal tibial osteotomies in putting off the need for a total knee arthroplasty are approximately 75% to 80% at 10 years, with some studies reporting that 65% of patients up to 20 years have relief of their knee pain. The advantage to reshaping the tibia and not requiring a partial or total knee arthroplasty is that one can continue to participate in higher level activities, such as climbing, hiking, and hunting, without fear of having their prosthesis wear out. We certainly do not advocate that patients go back to high-impact activities, such as long distance running, unless they are recognizing that they do run the risk of having their knee wear out sooner from the proximal tibial osteotomy surgical procedure.
The use of proximal tibial osteotomies in the United States is increasing, mainly due to the higher rates of arthritis that are developing in the medial compartment of patients who have had their medial meniscus resected. The improving outcomes that were seen in patients who have these are also driving the increased use of proximal tibial osteotomies.
What is the Recovery After Proximal Tibial Osteotomy?
Postoperatively, patients who have a proximal tibial osteotomy usually are partial to non-weightbearing for the first 8 weeks after surgery. X-rays at that point are obtained to determine if the osteotomy is healing sufficiently to be able to allow for initiation of weightbearing. Progression of weightbearing is usually carried out at one-quarter body weight per week until the 3-month point, at which point new x-rays are obtained. If the new x-ray shows sufficient healing, the patients can wean off of crutches when they can walk without a limp at that point in time. In general, the recovery from a proximal tibial osteotomy can be quite rapid at that point in time because one does not have to worry about ligament healing or other issues and working on a progressive quadriceps strengthening program with a stationary bike and elliptical machine can also allow one to get back to activities sooner. We have found that most of our patients reach their maximal improvement after an osteotomy, assuming that the strength is restored, at about 6 months postoperatively and this level of improvement seems to stay present for at least 5-7 years postoperatively, and probably longer.