One of the first things a physician does is to inspect the knee. Abrasions, lacerations, previous scars, swelling or prominences are important to evaluate. Swelling around the knee can be either due to causes outside the knee (extraarticular) or causes from inside the knee (intraarticular). In most circumstances, a physical exam can determine whether the swelling is from inside or outside the knee.
Localized swelling is most often due to an injury. It may indicate a tear of a collateral ligament, bruise or other localized injury. There may also be swelling around the pes anserine bursa, a Baker’s cyst, which is swelling from inside the knee which leaks out through a hole on the back of the knee between the direct arm of the semimembranosus tendon and the medial gastrocnemius tendon, or other causes.
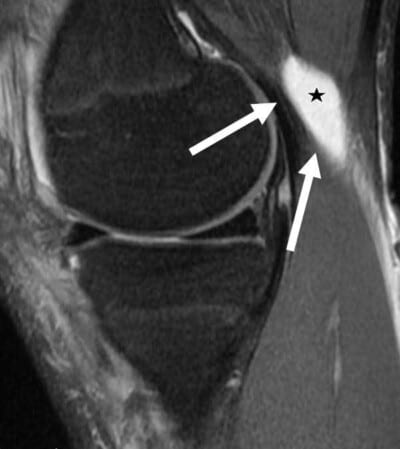
A Baker’s cyst of the posterior aspect of the knee is visualized on the sagittal MRI scan. A Baker’s cyst forms between the direct arm of the semimembranosus and the medial head of the gastrocnemius. It is not a true cyst, but rather an area where up to 90% of people have a hole in the back joint lining in the back of their knee and fluid from the fluid leaks out the back of the knee through this hole. There is no true cyst lining here, and the size of the cyst usually depends upon the amount of swelling that occurs in the front of the knee. Treatment of a Baker’s cyst usually means treating the problem in the front of the knee to decrease the joint swelling.
CLICK IMAGE TO ENLARGE
An intraarticular knee effusion can be due to bleeding from an acute injury, gout or pseudogout, swelling from arthritis, infection or other causes. It is important to determine whether the knee is warm, red, or painful to also evaluate intraarticular swelling. Intraarticular knee effusions usually result in the loss of the normal contour of the extensor mechanism, with fullness along the edges of the inside and outside of the quadriceps tendon. Large effusions may also cause the patella to be more mobile. Sometimes, a fluid wave can be created by palpating one side of the joint and feeling the fluid wave hit ones fingers on the other side of the joint. This is not as useful as other means to evaluate for an effusion because these are usually pretty obvious. One of the best ways to evaluate subtle effusions is to have the patient maximally flex their knee and compare one side to the other to see if there is any obvious fluid protrusion along the edges of the patellar tendon.