What is the Common Peroneal Nerve?
The common peroneal nerve is a branch off the sciatic nerve which mainly supplies sensation to the top of the foot, the outside of the leg, and the web space between the great toe and the 1st toe. It controls the ability for one to extend (lift up) the great toe, the lesser toes, and the ankle, and to move the foot outwards (eversion). The common peroneal nerve is one of the most vulnerable to entrapment or injury in the body because it passes about 2 cm below the lateral aspect of the fibula, where it is very subcutaneous.
What Causes Peroneal Nerve Irritation?
Irritation of the common peroneal nerve can occur from a direct or indirect injury, prolonged pressure such as sleeping against a car console with one’s fibular head against it, or due to instability such as instability of the proximal tibiofibular joint. In addition, it is one of the most commonly injured nerves when there is an injury to the lateral (fibular) collateral ligament, posterolateral corner of the knee, or when there is a knee dislocation.
Because the common peroneal nerve is so subcutaneous, it can get caught up in scar tissue after injury and become irritated. The symptoms from this can range from numbness with prolonged activities, weakness of one’s ankle, a foot drop, or any combination of these. In particular, when one has scar tissue entrapment or a proximal tibiofibular joint instability problem, increasing one’s activities can cause some irritation of the nerve with some shooting pains on the outside of the leg down into the top of the foot.
It is very important to ensure that there are no other causes of common peroneal nerve irritation, which can include lumbar disc herniations, axonal damage to the sciatic nerve after a nerve block, or other sources that are closer to the spine.
How to Diagnose Common Peroneal Nerve Entrapment
A diagnosis of a common peroneal nerve entrapment is almost always based upon a physical examination. Palpation of the nerve where it crosses the fibular head, or slightly posterior to this, can cause zingers to go down the leg, which is called a Tinel sign. If this reproduces the patient’s symptoms, it can indicate that the common peroneal nerve is irritable and may be encased in scar. Nerve conduction tests or EMGs can be obtained, but these only tend to show positive results with more severe nerve injuries and I have seen patients with disabling pain who have normal EMGs and nerve conduction studies.
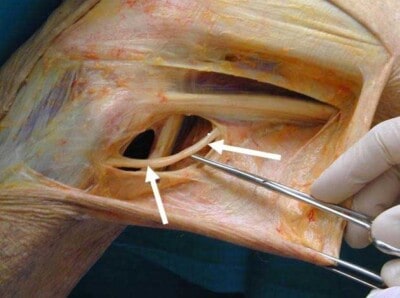
Photograph of a knee demonstrating a scar tissue release around the common peroneal nerve. Common peroneal nerve entrapment can occur due to a direct blow or by compression and the compression can cause numbness and tingling, or even weakness, down the affected distribution of the common peroneal nerve on the outside part of the leg and the top part of the foot. In addition, posterolateral corner injuries can have up to a 15% of incidence of a common peroneal nerve injury, so a common peroneal nerve neurolysis is almost always performed when a patient has a posterolateral corner injury to remove the scar tissue around it and minimize the risk of a footdrop postoperatively due to swelling.
CLICK IMAGE TO ENLARGE
How to Treat Common Peroneal Nerve Entrapment
The treatment for a scar tissue entrapment of the common peroneal nerve is to perform a common peroneal nerve neurolysis. This involves making an incision above the long head of the biceps femoris and the fibular head and then gently dissecting down through the scar tissue posterior to the biceps femoris tendon. In patients who have had injuries, this is a very meticulous portion of the surgery because commonly the nerve has been stretched before and may be in a different position than it should be normally. Therefore, one has to go slow and steady to find the nerve or remove the scar tissue around it. In addition to removing the scar tissue around it, it is felt that releasing the peroneus longus fascia, which can be a thick band that crosses the nerve, also is important to ensure that the nerve does not become irritated once again from scar tissue due to swelling or other means after surgery.
What is the Recovery Following Common Peroneal Nerve Entrapment?
We generally have patients remain toe-touch or non-weightbearing for 6 weeks to allow the scar tissue to quiet down around the nerve prior to increasing activities. The overall success rate for a common peroneal nerve neurolysis is believed to be about 75%, and if the nerve does recover initially and then develops scar tissue again, the second time around the success rate can be less.
Issues that we have seen that seem to make the nerve remain irritable are incisions placed below the biceps, which tend to make the skin and scar become more adherent to the nerve, or in patients who may have other associated instabilities that are not concurrently reconstructed, such as lateral collateral ligament tears or proximal tibiofibular joint instability issues.