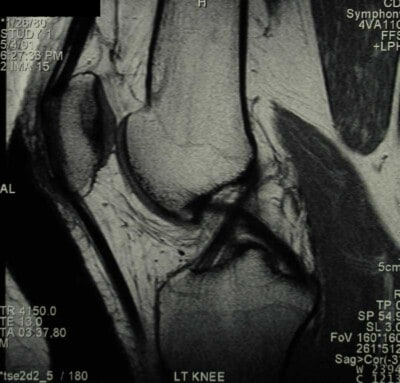
Anatomy of the Knee
The knee is one of the largest and strongest joints in the human body. Vital for multi-directional movement, the knee connects the thigh-bone (the femur) to the leg bone (the tibia). Most of this connecting mechanism is accomplished through ligaments.
Description of Ligament Knee Injuries
Ligaments are made up of strong, dense connective tissue and are crucial to maintaining knee stability. They are what allow the knee to perform movements such as walking, bending, running, turning, pivoting, etc. There are four main ligaments that stabilize the knee:
- The anterior cruciate ligament (ACL) and the posterior cruciate ligament (PCL): These ligaments are located on the inside of the knee and form an “X” in order to prevent the knee joint from sliding back and forth (up and down).
- The medial collateral ligament (MCL) and the lateral (fibular) collateral ligament (FCL or LCL): These ligaments are located on the sides of the knee and prevent the joint from moving side-to-side.
Knee ligament injuries that involve a ligament tear are very common, especially among athletes. Soccer, football, basketball, skiing and gymnastics produce the most knee ligament injuries. While most ligament injuries involve a single ligament, such as an ACL tear or MCL tear, when a major force or trauma is placed on the knee, multiple ligaments can be affected. For example, motor vehicle accidents, a hard crash on snow skis or a severe tackle on the football field can all result in complex knee injuries.
When multiple ligaments of the knee are injured, oftentimes, other problems are occurring such as a dislocated knee or a fracture. Special attention will be needed by an orthopaedic surgeon to surgically reconstruct the tears of the various ligaments.
Have you sustained a multi-ligament knee injury?
There are two ways to initiate a consultation with Dr. LaPrade:
You can provide current X-rays and/or MRIs for a clinical case review with Dr. LaPrade.
You can schedule an office consultation with Dr. LaPrade.
(Please keep reading below for more information on this condition.)
Treatment for Multi-Ligament Knee Injuries
A careful clinical exam and the use of stress x-rays are very useful, especially when there is a chronic injury or in the case of traumatic knee injuries, where it is difficult to determine whether a side-to-side laxity is due to a medial or posterolateral corner injury. In these injuries, a patient’s alignment must be assessed, especially for chronic injuries, and a high quality MRI scan should be obtained to look for any concurrent cartilage or meniscus injuries.
Non-operative treatment may be suggested initially when there is a concurrent ACL and medial sided knee injury to allow the MCL to attempt to heal first, or if there is a concurrent grade I or grade II injury of the medial or lateral side structures of the knee with a cruciate ligament injury. When there is more than this amount of instability present in the knee, Dr. LaPrade will usually recommend a concurrent multiple ligament reconstruction. The basic principles followed for multi-ligament knee injuries are to attempt a secure and well-positioned anatomic reconstructive procedure, whereby one can start early range of motion to minimize the chance of the patient developing stiffness and scaring around the knee. We believe this ultimately leads to decreased function and osteoarthritis and our goal is to help patients return to their highest level of functioning.
Post-Op
As mentioned previously, it is essential to have a concurrent well-guided physical therapy program following a multi-ligament knee injury reconstruction. Patients must achieve full knee extension as soon as possible, and work on quadriceps activation and edema control. It is also important to obtain 0-90° of knee flexion within the first two weeks. Further motion is obtained between weeks two and six and patients are usually kept non-weight bearing for the first six weeks postoperatively.
Recovery after complex knee injuries require 9-12 months of postoperative rehabilitation before returning to full activities. Allowing the ligaments to heal properly and to restrict the patient from returning to activities too soon will decrease the risk of having the reconstructed graft fail or develop fatigue and endurance problems and have the operative knee or the contralateral opposite healthy knee (re)injured.
Related Studies
- Effects of Grade III PLC Injuries on ACL Grafts
- Effects of PLC injuries on PCL Grafts
- Effect of Tibial Postioning on the Diagnosis of PLC Rotatory Instability in the PCL Deficent Knee
- sMCL – Anatomic Augmented Repair vs Anatomic Reconstuction
- Biomechanical Comparison of Anatomical Single and Double Bundle ACL Reconstruction
- Double Bundle PCL Technique and Outcomes
- Outcomes and Surgical Technique of Acute Grade III and Combine PLC Injuries
- Varus Stress Radiographs
- Correlation of Valgus Stress Radiographs
- Kneeling Stress Radiographs for Evaluation of Posterior Knee
Multi-Ligament Knee Injury FAQ
1. What is a Multiple Ligament Knee Injury?
A multiple ligament knee injury involves an injury to at least two of the four main ligaments of the knee. These include the ACL, PCL, MCL (and its components), and the posterolateral corner of the knee (where the FCL/LCL, popliteus tendon and popliteofibular ligament are all considered important structures on the outside of the knee). A knee dislocation is considered a severe multiple ligament knee injury.
2. How does one Diagnose a Multiple Ligament Injury?
Some multiple ligament knee injuries present with a dislocated knee, some present after having dislocated and self-reduced on the field or after an injury, and some never really dislocate but have complete tears to multiple knee ligaments. Thus, it’s important to discuss with the patient and see if they can recall any particular injury pattern that they could feel at the time of their knee ligament injury or if they felt their knee was out of position.
The most important way to initially diagnose these injuries is to review a thorough history with the patient to recall that their knee felt that it dislocated and slipped back in. It’s important to determine if this was solely their kneecap joint where there was a patellar (kneecap) dislocation or if it was the complete knee joint itself slipping out of place. These injuries are considered to be very severe and potentially limb and life threatening. Thus, assessing for this and insuring that the patient’s knee function is intact, including both the status of the pulses to ensure that the artery is not injured as well as their sensation to ensure that there are no nerve injuries present is important. Nerve injuries can be present in many multiple ligament knee injuries, especially injuries to the common peroneal nerve where 15% or more of patients with an injury to their posterolateral knee have some type of injury to this nerve.
Next, one needs to perform a complete physical exam to determine where the injury pattern would be when there is a multiple ligament knee injury. The best test to determine the integrity of the ACL is to perform the Lachman test to assess if there is any significant increase in anterior tibial translation when the knee is flexed to between 20 and 30 degrees. The pivot shift test also assesses the integrity of the ACL and the amount of anterolateral rotation, but this test is often hard to perform in patients with an acute knee injury. The posterior drawer test is important to assess the integrity of the PCL and the amount of posterior tibial translation that a patient may have from a PCL injury. This test is performed with the foot in neutral rotation and the knee flexed to 90 degrees and determines the amount of posterior shifting of the knee that occurs with a PCL tear. In general, a PCL tear by itself will have the knee slip back to the point where the femoral condyle is even with the tibia, whereas when the tibia slides back behind the condyles, it usually means that there is a combined PCL and posterolateral corner (or other pathology like the MCL) injury present.
Assessing for an injury to the MCL involves the assessment of gapping on the inside part of the knee with the valgus stress test in both full extension and at 30 degrees of knee flexion as well as the dial test and anteromedial drawer test to look at anteromedial rotation that can occur with these injury patterns. With knees that gap in full extension, this usually indicates a very severe medial sided knee injury, and these MCL injuries have a much lower chance of healing without surgery. If the knee does not gap in full extension, and it does gap open to a valgus stress at 30 degrees of knee flexion, these MCL injuries usually have a much higher chance of healing because they are either not completely peeled off the tibia or the posterior oblique ligament is still attached on the inside part of the femur (thighbone). Assessment of lateral compartment gapping is best performed with a varus stress test to see how much gapping there is compared to the contralateral side and assessing the amount of rotation that occurs can be assessed both with the dial test at 30 and 90 degrees of knee flexion and the posterolateral drawer test. Finally, assessing any increases in heel height can be important to determine if there is a posterolateral corner injury. These injuries may be somewhat difficult to determine in acute situations because of pain, but any increases in centimeters of heel height compared to the contralateral side should make one concerned that there is a combined FCL (LCL) and ACL tear present.
3. What is the Best Treatment for a Multiple Ligament Injury?
In order to determine the best treatment for a multiple ligament knee injury, it’s important to recognize the rather significant advancements that have been made in treating these pathologies over the last two decades. Prior to the mid-1990s, it was still recommended that these patients be treated either without surgery or with casting because surgical techniques and fixation devices were inferior at that point in time. In addition, more recently, looking at anatomic-based reconstructions rather than repairs has also improved patient outcomes. Finally, many of these injuries were treated with casting or immobilization for two to six weeks after injury because surgeons felt that the repairs or reconstructions were at a higher risk of stretching out. Early motion has been advocated by our team for over two decades, whereas it has only been accepted as the current standard of care in the last two to three years at some centers. It has also been documented that early range of motion is better than delayed range of motion and patients have both a higher overall functioning level with early range of motion and also a much lower risk of developing a stiff and nonfunctioning knee (arthrofibrosis).
4. What is the Current Standard of Care for a Multi-Ligament Knee Injury?
The current standard care for a multi-ligament knee injury is to operate earlier rather than later, to perform reconstructions rather than repairs for the main static stabilizers and to start physical therapy with early range of motion as soon as possible (preferably on postoperative day one). While these anatomic-based surgical principles may seem simple, they were only universally advocated as the standard of care within the last three years. In contrast, our group has advocated this approach for almost 20 years, and our publications have documented that our clinical outcomes are superior to returning patients back to high levels of activity when these protocols are followed compared to some of the older protocols.
Thus, early surgery with anatomic-based and biomechanically validated reconstructions of the ACL, a double bundle PCL, an MCL with or without a posterior oblique ligament repair or reconstruction, and a posterolateral corner reconstruction, which can be either an anatomic reconstruction of the FCL/LCL or a complete posterolateral corner reconstruction, are able to restore stability to the knee, allow for early and safe range of motion, and provide significantly improved outcomes for these patients.
We have found that overall even though these injuries are often quite severe, in the vast majority of cases where they are treated with these principles, we were able to restore the patients back to functioning levels seen historically with isolated ACL reconstructions. A review of our many papers looking at quantitative anatomy, improved ways to diagnose these injuries, new biomechanical studies based on the redefined anatomy, and the development of anatomic-based reconstructions for the ACL, PCL, posterolateral corner, MCL, proximal tibiofibular joint, popliteus tendon and multiple variants of meniscus repairs are located within the research section of our website so that one can see these new publications. Almost all of them are published in the highest impact orthopedic journals, which helps to validate many of our procedures. In addition, the banners on several of these high level peer review publications note which ones were selected by our peers as nationally and internationally-based research award winners because of the novel and new approach to treating these pathologies.
5. What is Knee Pseudo-Instability?
Pseudo-instability of the knee is important to recognize. In general, this is usually because a patient has arthritis of one compartment of the knee which can make the knee swing side-to-side and feel like it is unstable on clinical exam. In addition, when these patients ambulate, they can have a wobble to their knee which we call a varus or valgus thrust gait. It’s important to examine these patients carefully to ensure that one is feeling if there is pseudolaxity or gapping at the joint line and to validate that the pseudolaxity is occurring on either the inside or outside of the knee. The best way to diagnose pseudolaxity is to obtain long leg x-ray to see if one is bow-legged or in a knock-kneed position (varus versus valgus alignment) and also to look at standing x-rays including a standing Rosenberg view to see if the patient does have significant arthritis when it feels like the patient has pseudolaxity. If one is concerned that there is a defined amount of arthritis and also concurrent gapping of the affected compartment, bilateral varus or valgus stress radiographs will provide a confirmatory answer to this in terms of the amount of gapping that is present on the normal compared to the contralateral normal knee.
6. Can one have Knee Instability but no Pain?
Yes, one can have knee instability but no pain. Pain can often be caused by arthritis, pre-arthritis whether some early damage forming to the cartilage, or a meniscus tear. In particular, PCL tears are known not to cause a lot of pain, whereas the underlying cartilage may slowly and progressively wear out over time and develop arthritis. It has been reported that patients with chronic PCL tears have a significant amount of arthritis develop within an average of seven years after their injury. This slow and subtle development of arthritis is usually in the patellofemoral (kneecap) joint and the medial compartment of the knee in these patients. Thus, we recommend that patients who do have knee instability may not have a lot of pain consider an anatomic-based reconstruction to minimize the risk of the development of arthritis further down the road.
7. What is Side-to-Side Knee Instability?
Side-to-side instability of the knee happens when there is an injury to structures of the knee either on the outside or inside of the knee. In this circumstance, when one goes to plant toward the side of the injury, the joint line may gap open and the joint may feel unstable. In addition, one may have that feeling of side-to-side instability even with normal walking activities. In patients with long-standing knee pain, they may appear to have side-to-side instability, but they actually have pseudolaxity because of bone-on-bone arthritic changes and the knee collapsing down rather than gapping open with these mechanisms.
8. What Causes Knee Instability when one is Walking Down Stairs?
Many things can cause a feeling of knee instability when going down stairs. If one has weakness of the quadriceps, they can pinch the tissues that are along the kneecap joint (retropatellar fat pad) and have a sensation of giving way. This is usually due to quadriceps inhibition.
Patients who have true instability where they feel like their knee is sliding forward when going downhill, down inclines, or down stairs most commonly have a PCL tear which is the cause of this. If one has had it for a while, using a dynamic PCL brace such as the PCL Rebound brace, may help to hold one’s knee in a normal position and confirm that that is the underlying problem. In many of our patients who present with chronic PCL tears, we will place them into a Dynamic PCL brace to see if their knee feels better. In almost all cases, this confirms to the patient that the PCL tear is causing them a significant amount of problems and most proceed with having a double bundle PCL reconstruction to reconstruct the torn PCL and eliminate this feeling of instability when they are going down inclines or down hills.
9. Can one have Back Pain Associated with Knee Instability?
If one is limping due to knee instability, it will often throw off the mechanics of the sacroiliac joint. In these patients, they can also have weakness of their hip abductors which can lead to a positive Trendelenburg sign. When this is chronic, these patients often have a sensation of back pain which is most likely localized to their SI joint in these patients, as well as weak hip abductors and some patients will also have trochanteric bursitis. Working on eliminating the cause of limping as well as working on a hip abduction strengthening program can often be effective at eliminating the “back pain” in these patients.
10. What are the Different X-ray and MRI Types for Multi-Ligament Instability?
It’s important to look at standard knee x-rays to ensure that there are no fractures when one does have a multi-ligament knee injury. Often, patients with tibial plateau fractures may have other associated ligament tears and patients who present with instability need to be assessed to ensure they don’t have a concurrent fracture of their plateaus. Specifically, avulsion fractures of the fibular head, lateral capsule (Segond fracture), or other avulsions such as the tibial eminences (which may indicate an injury to the ACL) or a PCL avulsion fracture posteriorly may also be assessed.
Looking at one’s alignment on a long leg x-ray is important as well as assessing the kneecap on a 45-degree x-ray can help determine if one has any underlying arthritis or any subluxation of their patella.
In addition, patients should have varus, valgus and posterior knee stress x-rays if there is any concern about collateral ligament injuries or a PCL tear. It’s important that this objective information be obtained in these circumstances so that one can see how much instability they have and that the surgical procedure ultimately work for them after surgery. We strongly recommend that all patients with multi-ligament knee injuries have stress x-rays whenever possible to ensure the best preoperative diagnosis of the pathology.
Moreover, all patients who have multi-ligament knee injuries should also have a concurrent MRI scan. In acute injuries, the MRI can be very precise at determining the status of the underlying cartilage, if there are any peripheral, radial or meniscus root tears, and also looking at potential avulsions of key structures such as the biceps femoris, medial and lateral capsules, and the posterior oblique ligament. It is also very effective in acute situations at diagnosing ACL, PCL and MCL tears, whereas tears of the LCL that are more subtle may require stress x-rays to ensure that the correct diagnosis is obtained. In patients with chronic multi-ligament injuries, it can be very difficult to determine if thickening seen in the MCL, PCL or posterolateral corner structures is a healed ligament or if it is a very stretched out and nonfunctional ligament without the use of stress x-rays. In general, assessment of the articular cartilage, meniscus and ACL can be effective either with acute or chronic injuries.
11. Can one Self-Diagnose a Multi-Ligament Knee Injury?
In general, we would not make a recommendation for a self-diagnosed injury, but relying on one’s history can often be useful to determine if you potentially have a multi-ligament knee injury. If one has a knee injury during a sporting event such as on the field with football, soccer or on the court with basketball, or while skiing, one may have a history that can help determine if you do have a multi-ligament knee injury. In general, in most of these circumstances, unless there is severe pain patients can often try to get up and walk it off. In the process of doing this, if one feels side-to-side instability or a severe rotation of the knee, one has to be concerned that there may be a multi-ligament knee injury in these circumstances.
It’s also important to be assessed to make sure that one doesn’t have a concurrent fracture, and this usually presents itself as rapid swelling in the knee because of the blood that forms from the fracture. In more chronic circumstances, if one does feel side-to-side instability or significant difficulty where one’s knee feels unstable going down hills or down inclines, one should be concerned that they may have a multi-ligament knee injury and we would recommend being assessed by a physician with a good clinical exam and stress x-rays to best document this pain.
12. What are the Best Braces for Knee Instability?
It is important to determine what type of knee instability one is treating when determining what the best braces may be. Certainly, some of the more modern knee braces are very affective at preventing knee instability. In particular, Dynamic PCL braces have only been developed over the last decade and they have been found to be extremely effective at preventing the negative affects due to gravity from causing a PCL injury, repair, or reconstruction to stretch out and develop recurrent instability due to the effects of gravity. Thus, Dynamic PCL braces, such as the PCL Rebound brace, are essential for the treatment of PCL reconstructions in modern PCL surgery techniques.
In addition, the use of a hinged knee braces to prevent side-to-side instability for patients who have medial or posterolateral corner surgery are essential. These braces help to provide stability of the knee, and allow one to increase their activities without having to worry about a significant risk of re-injury to their reconstructed ligaments if they do stumble and fall. These are the main functions of these braces.
The development of an ACL Dynamic brace is ongoing. In particular, the ACL Rebound brace has been developed to treat ACL reconstructions that are at high risk. These include patients who have hamstring reconstructions that have a higher risk of stretching out, patients who have increased heel height (genu recurvatum), ACL allograft reconstructions which utilize a donor rather than one’s own tissue for the graft, and revision ACL reconstructions. In all of these circumstances, having a Dynamic ACL brace to push the knee posteriorly intuitively should improve patient’s outcomes and decrease the risk of failures of these reconstructions going forward.
Other unique uses of braces may be unloader braces in patients who have particularly complex surgeries, especially for revision collateral reconstructions, to push the knee towards the area of the injury pattern to minimize extra stress on the reconstruction grafts. For example, a patient that has a revision posterolateral corner reconstruction may benefit from the use of a medial unloader brace which pushes the knee towards the outside of the knee and helps to unload the healing revision reconstruction. Revision reconstructions in general have less healing potential because of disruption of the original blood supply and take longer to heal; thus, the use of an unloader brace may be beneficial in protecting that graft and given them the best chance to have an improved outcome for that particular patient.
13. What Causes Clicking after a Multi-Ligament Knee Injury or after Multi-Ligament Knee Surgery?
Nonpainful clicking of the joint can often be due to some swelling of the joint causing decreased viscosity. In this circumstance, the swelling in the region can make the joint fluid less able to let normal structures slip, and it may catch and cause clicking. It has been reported that the normal viscosity of the joint fluid is one-sixth that of ice-on-ice, so any swelling from an injury can disrupt this normal viscosity and cause normal tissues to catch instead of being able to glide normally.
Often, when one does have nonpainful clicking after an injury or after surgery, one almost always gets better as one gets stronger. Whether this is because the swelling decreases because ones strength improves, or if the tissues are better pulled out of the way when one achieves improved strength, is unknown, but in general most causes of clicking occur within the first two to four months after surgery and improve over time as one’s swelling decreases and strength returns after surgery.
14. What Type of Knee Instability Happens with an LCL Tear?
The LCL, or FCL, is located on the outside part of the knee. It prevents the knee from gapping towards the outside. Most isolated tears of this ligament have very minimal swelling and because there is minimal swelling there is also minimal pain. Therefore, in high school and intercollegiate football players, patients often present to a physician’s office several weeks after their original injury with problems with feeling a side-to-side instability.
Because the outside part of the knee is inherently bony unstable because of the two convex surfaces of the lateral femoral condyle and lateral tibial plateau, there is a very low chance that injuries to this structure will heal without some looseness in most patients. We have validated this in several natural history animal studies where we cut and posterolateral knee structures and they did not heal and have also validated that it is the bony geometry that makes the LCL have a low chance of healing.
Thus, some patients with LCL tears have minimal pain, rehabilitate and get stronger and then when they go back to activities they notice that they can’t plant and pivot towards the knee that has the LCL tear. This is because the knee will have side-to-side instability. It is has not been uncommon that parents will bring athletes in to be evaluated when they complain of side-to-side instability because sometimes plays were developed by their coaches to avoid running to that side rather than recognizing that the players had an underlying injury which should have had medical attention.
Probably the most important thing to recognize is that because an LCL tear does not hurt, doesn’t mean that it is not a severe injury. Most of these patients will have side-to-side instability which can lead to meniscus tears and arthritis on the inside part of the knee if they are not treated. Thus, when does feel the side-to-side instability, it is important to be evaluated and treated soon because surgical reconstruction of the LCL/FCL is one of the more successful surgeries around the knee. Diagnosing and treating it soon after injury gives one of the best chances in restoring the knee function best over long term.
15. How does one Diagnose a Chronic PCL Tear?
It is not uncommon for patients to present with chronic PCL tears in our practice. This is because when the PCL does tear, there can be often very minimal swelling in the knee when it is an isolated injury. In addition, the PCL tends to heal over time, but often the healing occurs in a loose position if it is not recognized and treated with a Dynamic PCL brace immediately after injury. Thus, these patients will ultimately present with difficulty in going down stairs or down inclines or it can present with pain in the front of their knee due to the fact that the tibia is slipping back posteriorly and the retropatellar fat pad gets pinched.
When these patients present to our clinic and their clinical exam demonstrates they have a positive posterior drawer test, we will obtain PCL stress x-rays to objectively determine the amount of posterior tibial translation that occurs. When the patient has 8 mm of increased posterior tibial translation on their injured side compared to the contralateral side, it will indicate that the PCL is completely torn and basically nonfunctional, even if the MRI scan shows that it is “healed” and intact because effectively it is nonfunctional. This is because the PCL stretches out like a piece of taffy and just cannot become tighter again. In addition, our biomechanical studies have shown that when there is only a tear of one of the two bundles of a PCL, the PCL stress x-ray should be at most 3 to 4 mm. Thus, a patient would presents with 6 or 7 mm of increased posterior tibial translation also has to be evaluated for a high grade partial tear of their PCL which maybe causing decreased function.
In almost all of these patients who present with a chronic PCL tear, we help them to confirm the disability from their diagnosis by placing them into a PCL Rebound Dynamic brace. This brace helps to hold the tibia in a more normal position and prevent the knee from slipping posteriorly. We have found that it is very affective to demonstrate the patients that when their fat pad is not pinched, or in more chronic cases that the kneecap arthritis is less stressed, that they have minimal pain and also that they can function going downhill and down inclines. Over 90% of our patients who presents with chronic PCL tears who are placed into this brace want to proceed with PCL reconstruction surgery because the brace helps to validate that the complete PCL tear is their underlying pathology and that they can get better with having a stable knee via a PCL reconstruction.