What is an ACL Injury?
The anterior cruciate ligament, or ACL, is the most important ligament of the knee to prevent the knee from sliding forward or rotating anterolaterally. Patients who sustain an ACL tear often have problems with twisting and turning activities, such as in playing football, soccer, or skiing, and will often require an ACL reconstruction to provide stability to their knee.
In addition to its stability role in the knee, the ACL also provides protection for the menisci of the knee. When the knee continues to have instability episodes, it is not uncommon to have either the medial or lateral meniscus tear. However, when menisci tear there is much higher risk of the development of osteoarthritis. Because of this, Dr. LaPrade usually recommends ACL surgery and that an ACL reconstruction be performed in young or otherwise active patients and in almost all patients who report instability with twisting or turning activities.
An ACL injury is classified by the amount of injury to the ligament:
• Grade I: a partial ACL tear
• Grade II: near complete ACL tear
• Grade III: a complete ACL tear – the ligament is non-functional
Depending on the patient’s age, activity level and grade of tear will determine the correct treatment option.
Description of ACL Reconstruction
An ACL surgery requires precise knowledge of the anatomy of the knee, attachment sites of the ACL and knowledge on the other ligaments and structures of the knee. If one fails to replace an anterior cruciate ligament at its correct attachment sites or if other concurrent injuries are not treated, there is a much higher risk of failure of the ACL graft.
While there are two bundles of the ACL, the anteromedial and posterolateral bundles, there is still controversy as to whether both should be reconstructed as a single ligament or as two separate ligament grafts. While the double-bundle ACL reconstruction technique appeared very promising initially, many research groups, including ours, have significantly narrowed the indications for double-bundle ACL surgery and found there is very little difference between a single and double-bundle ACL reconstruction for the vast majority of patients.
The most important technical issue is to have the ACL reconstruction graft placed in the correct position. On the tibia (shinbone), the tunnels should be in line with the posterior margin of the anterior horn of the lateral meniscus. On the femur (thigh bone), the reconstruction tunnel should be placed at the midpoint of the attachment bundles of the anteromedial and posterolateral bundles, with the main portion of the reconstruction tunnel being posterior to the lateral intercondylar ridge (resident’s ridge).
A large number of ACL reconstruction graft failures are in those patients who have the graft placed too posterior (central) on the tibia with an inability to control rotation of the knee or too anterior on the femur (anterior to resident’s ridge) or too central on the femur (effectively only reconstructing the anteromedial bundle), which leads to either stretching of the reconstruction graft or failure to control knee rotational laxity.
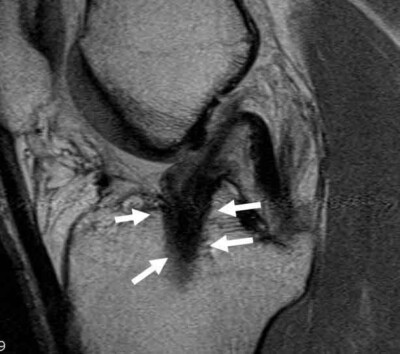
ACL Graft Placed Too Central On The Tibia
Sagittal MRI scan demonstrating an anterior cruciate ligament graft placed in a nonanatomic position on the tibia. The central position on the tibia does not allow for rotational control, so these patients may have problems with instability with twisting, turning and pivoting.
CLICK IMAGE TO ENLARGE
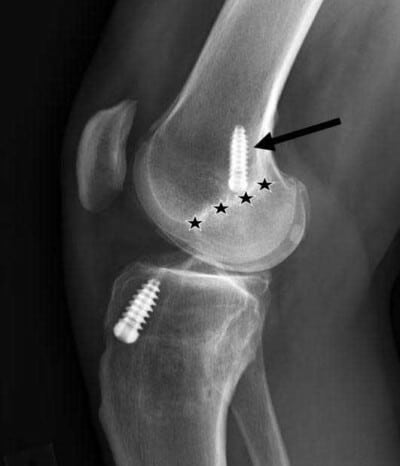
ACL Tunnel Too Central
Lateral knee x-ray demonstrating a central position of the ACL reconstruction graft on the femur. In this position, the fixation device is located above Blumensaat’s line, which indicates that the graft is placed centrally. These grafts often have a negative Lachman’s test but patients often will have a positive pivot shift and have instability with twisting, turning, or pivoting activities.
CLICK IMAGE TO ENLARGE
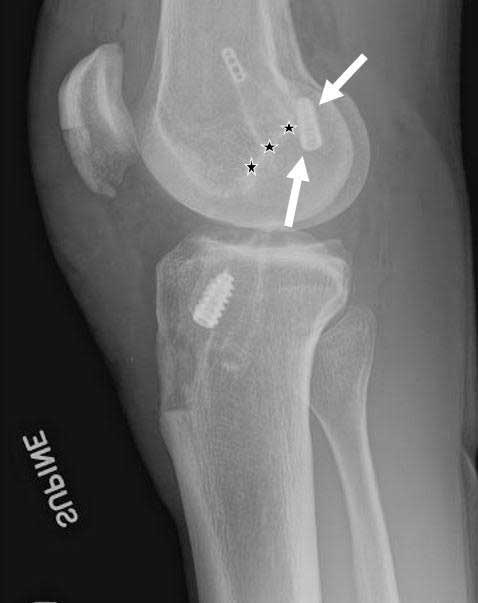
Lateral Knee X-ray of ACL Reconstruction Tunnels
Lateral knee x-ray demonstrating a central position of the ACL reconstruction graft on the femur. In this position, the fixation device is located above Blumensaat’s line, which indicates that the graft is placed centrally. These grafts often have a negative Lachman’s test but patients often will have a positive pivot shift and have instability with twisting, turning, or pivoting activities.
CLICK IMAGE TO ENLARGE
ACL Surgery Technique
The technique of ACL reconstructions has changed dramatically over the last decade in orthopaedics. ACL reconstruction grafts performed prior to 5-10 years ago were usually placed more centrally on both the tibia and femur and many of these patients have continued problems with rotation instability. This problem became recognized through extensive clinical and biomechanical research and the surgical technique has currently changed dramatically to where the reconstruction tunnels are now placed more anatomically to provide better stability to the knee.
Dr. LaPrade’s primary surgical reconstruction technique involves using a patellar tendon autograft (from the patient’s own tissues) during ACL surgery. The reconstruction tunnel is drilled at the anatomic attachment site of the ACL on the tibia and a closed socket tunnel is drilled at the ACL attachment site on the femur. The patellar tendon graft is pulled into the joint and fixed in place with titanium interference screws. Dr. LaPrade utilizes one incision for this surgical technique, as well as an autograft to place it in the correct position. The utilization of fewer incisions results in less pain post-operatively for the patient, while the use of the autograft allows the patient to return to activities sooner with a lesser risk of reconstruction graft failure.
Patellar tendon allografts (donor grafts) or soft tissue graft material may be required in patients with open growth plates or in older patients (women greater than 40 years, men greater than 45-50 years) due to the desire not to have any bone across an open growth plate and for older patients to have a strong enough graft. Cadaver grafts can be larger than ones harvested from one’s own knee and it is well known the patellar tendon and the other grafts around the knee are approximately three times weaker in someone who is 60 years of age compared to someone who is 20 years of age.
Post-Operative Protocol for ACL Reconstruction
It is absolutely essential for a physical therapist to be consulted and to work with one’s surgeon post-operatively following ACL surgery. Reactivation of the quadriceps mechanism, edema control, patella mobilization, maintenance of full knee extension and regaining knee motion are absolutely essential to obtaining optimal post-operative outcomes.
In our practice, we strongly suggest and require patients remain in the area to work with our physical therapists at for a minimum of 5-7 days post-operatively to make sure they are having appropriate care post-operatively and also so that their rehabilitation will advance to higher levels sooner.
Related Content
- Biomechanical Comparsion of Anatomical Single and Double Bundle ACL Reconstruction
- Femoral Cortical Suspension Devices for Soft Tissue ACL Reconstruction
- Biomech Comparison of Tibial Fixation for Soft Tissue ACL Grafts on the Tibia
- Functional ACL Bracing – Current State
- Effects of Grade III PLC Injuries on ACL Grafts
ACL Reconstruction FAQ
1. When to have ACL surgery after injury?
Athletes who have any difficulty with twisting, turning, or pivoting after an ACL tear should consider having their ACL reconstructed. This is because repeated twisting and turning mechanisms can damage both the cartilage in the joint and also the menisci. The medial meniscus is the most at risk to injury with an ACL tear because the medial meniscus takes over a lot of the function of the ACL when it is torn to prevent the knee from slipping forward. In addition, patients who may have a repairable meniscus tear at the time of their ACL tear should consider surgery to prevent the tear from becoming non-reparable. In general, most people who tear their menisci will be developing arthritis and having symptoms within 8-10 years after their ACL tear. Thus, one of the main reasons for the general public to consider having an ACL reconstruction is both to repair any meniscal tears which are repairable, and also to prevent meniscal tears from developing if their knee is unstable.
2. What is ACL reconstruction surgery?
ACL reconstruction surgery consists of replacing a torn ACL with another ligament or tendon. This can be from one’s own body (an autograft) or from a donor (an allograft). In an ACL surgery, tunnels are reamed at the normal attachment site of the ACL on both the femur and tibia and the graft is secured either inside or outside these tunnels. The type of graft from one’s own body and whether one should use a cadaver graft tissue or not can depend on multiple factors. This can include the patient’s age, if they have hyperlaxity, where they participate in contact sports, and other factors.
3. How is an ACL reconstruction done?
An ACL reconstruction is done by replacing the torn ACL with tissue that is placed at the normal attachment sites of the native ACL. This involves reaming a tunnel in the femur (posterior to the lateral intercondylar ridge) and also in the tibia (adjacent to the anterior horn of the lateral meniscus) and then securing the graft within those tunnels. There are multiple ways to secure the graft, and this can include fixation within the tunnels with metal or bioabsorbable/plastic screws or through a loop and button placed on the outside of the tunnels. In general, the fixation of the grafts is performed according to the way the surgeon was originally taught, with the gold standard being screws placed within the tunnels for patellar tendon grafts and looped sutures with cortical buttons or screws within tunnels for hamstring ACL reconstruction grafts.
4. When should an ACL be repaired?
The main time that ACLs can be repaired is when an ACL is torn with a piece of bone, usually off the tibia, which is much more common than when torn off the femur. In this circumstance, if there is not a lot of intrasubstance stretch within the torn ACL, the bony can be refixed at its normal attachment site and secured such that early motion can be started. In those instances where the tissue is not strong enough to allow early motion, there is a much higher risk of stiffness if immobilization is required after surgery.
In terms of a repair of the ACL, there are perhaps 10% of patients who may have injury only to the attachment site on the femur or tibia and sutures can possibly be placed in to do a repair. In those circumstances, research is still ongoing to try to improve outcomes because attempts at repairs in the literature previously have not shown good outcomes over time. Thus, more research is necessary to define better techniques to perform ACL repairs in those circumstances. It is important that these techniques be based upon good science and not on marketing by device companies because previous attempts at ACL repairs did not show failures until after two years after surgery.
5. How long is an ACL surgery recovery?
One of the most important things for preventing a retear of an ACL reconstruction is to ensure that the patient has gone through the proper recovery phase after surgery. In the past, many surgeons tried to get their patients back to full activities by 5 or 6 months. However, more recent data has suggested that waiting up to 9 months may be more advantageous in that the rate of retear goes down significantly after the 9-month timeframe for a return to activities after ACL surgery. In general, it is important to make sure that an athlete has a full return of proprioception, strength, agility, and endurance to minimize their risk of reinjury.
6. When I can run after ACL surgery?
The ability to return to running after an ACL surgery is dependent upon many factors. If the surgery is only the ACL, and there are no other ligaments or meniscus tears treated, and the cartilage surfaces are intact, then one has to go through a proper rehabilitation program first. In general, we feel that an athlete has to wait a minimum of 4 months after their ACL reconstruction return to running. In addition, they should have appropriate quadriceps strength. Our main goal is to be able to have them perform a single-leg squat with no bending of the knee inwards (valgus collapse) during the single leg squat. In these circumstances, if the patient has a good return of function, good motion, and does not have a valgus collapse when performing a single-leg squat, they are generally able to initiate a return to their running program at about the 4-month timeframe. This allows the quadriceps mechanism to be strong enough to prevent extra stress on the knee which can lead to knee swelling (effusions) and possibly damage the cartilage which would not be noticed until several years later.
7. What causes ACL reconstruction failure?
The number one cause of ACL reconstruction failure in all of the literature is improperly placed ACL grafts at the initial surgery. This can cause extra stress on an ACL reconstruction graft which can lead to its failure. In addition, a missed other ligament problem at th time of the ACL surgery, such as an MCL or a posterolateral corner injury, can also put significant stress on an ACL reconstruction graft, which can lead to its failure. Other factors that can cause an ALC graft to fail can include the lack of the posterior horn of the medial meniscus. This is because the posterior horn of the medial meniscus is the next structure that prevents the knee from sliding forward. In patients who may not have their medial meniscus, the ACL graft generally tends to be looser than in patients who do have their medial meniscus. Thus, in some patients, this can lead to the graft being overloaded and it can cause the ACL graft stretch out over time.
Other factors that can lead to ACL reconstruction failure are patients that have soft tissue grafts, such as hamstrings grafts, that have hyperlaxity. These patients who have a significant increase of heel height (more than 4-5 cm) have a much higher risk of having these grafts stretch out versus a patellar tendon graft. Other factors include patients with a large increase in their posterior tibial slope (sagittal plane tibial slope) which can cause an ACL graft to be overloaded and stretch out over time.
In my practice, where we perform over 75 revision ACL reconstructions a year, we find that a properly placed ACL reconstruction is the least common cause of failure. Therefore, patients who have a well-done ACL reconstruction and are exposed to sports activities, are the lowest numbers of athletes that we see that need a revision. Thus, it appears that when an ACL reconstruction is placed in the correct position and the patients appropriately rehabilitate themselves, the risk of an ACL reconstruction graft failure is much lower.
8. Patellar tendon ACL reconstruction versus hamstrings ACL reconstruction
Patellar tendon ACL reconstructions have been considered the gold standard now for almost 30 years. This is because they are the graft of choice for physicians who cover professional teams and for high level athletes; however, hamstrings grafts can also be considered to be appropriate for a large number of patients. Hamstrings grafts would be most appropriate for patients with open growth plates and in those patients who may have lower levels of activity desired after an ACL reconstruction. In general, a patellar tendon ACL reconstruction should not be performed in patients with significant arthritis of their kneecap joint, or may have had a previous patellar tendon harvest. Hamstring ACL reconstruction grafts should definitely not be considered in patients with a lot of hyperlaxity, such as in patients with a large heel height, because these grafts have been shown to stretch out over time.
In general, the large data base series have shown that the rate of retear is lower with a patellar tendon reconstruction compared to a hamstrings ACL reconstruction. However, a well done ACL reconstruction with either graft can be appropriate for the majority of patients.
9. Does ACL reconstruction lead to knee replacement?
ACL reconstruction by itself does not lead to the need for a total knee replacement. However, when one does have a knee injury, especially when one loses their meniscus tissue, they are at a higher rate for the development of osteoarthritis. In particular, patients who have ACL reconstructions have roughly a 50% chance of developing arthritis 20 years after their ACL reconstruction.
10. Can an ACL reconstruction fail?
The success rate of ACL reconstructions ranges from 60% to 95%, depending upon the graft used, the surgical technique used, and if all other patient-related pathologies, including their bony geometry have been addressed. In particular, one of the highest risk factors for an ACL graft failure is a patient who has a cadaver graft, called an allograft, when they are 25 years or less of age. The failure rate for these can be up to 40% or more in some series.
11. Can an ACL reconstruction be done twice?
ACL revision reconstructions are becoming more common because there are anywhere from 200,000 to 300,000 ACL reconstructions done each year in the United States. With all of the many factors that can lead to ACL reconstruction graft failure, anywhere from 20,000 to 40,000 ACL revision reconstructions may be performed per year in the United States.
12. Which ACL surgery is best for athletes?
There is no defined study which can definitively determine which ACL graft may be best for athletes. In general, it is felt that athletes put more stress on their knees and have higher demands than non-athletes. For this reason, most surveys of physicians who take care of professional teams recommend a patellar tendon autograft (from the same knee) as their graft of choice in these high-level and high-performing athletes.
13. What is an anatomic ACL reconstruction?
An anatomic ACL reconstruction means that the reconstruction graft is placed in the same location as a normal ACL is located. On the femur, this means that the graft is placed roughly midline along the lateral intercondylar ridge whereas the tibial reconstruction graft is placed essentially in line with the anterior horn of the lateral meniscus on the tibia.
14. What is a BTB ACL reconstruction?
A BTB ACL reconstruction is one that uses a patellar tendon graft. It is called a “BTB” graft because it takes bone off the patella, uses a strip of tendon, and then takes a piece of bone off the tibia. This graft has been documented in animal models to be the one that heals the fastest, with most bone plugs healing in their tunnels at around six weeks after surgery.
15. What is a double-bundle ACL reconstruction?
A double-bundle ACL reconstruction is one that uses two separate grafts to reconstruct the anteromedial and posterolateral bundles of the anterior cruciate ligament. Double-bundle ACL reconstructions were very popular about a decade ago, but clinical studies and biomechanical studies have not shown a great deal of difference between placing one graft in the center of the ACL attachment sites in the femur and tibia versus placing two grafts at the different attachment sites of these bundles on the femur and tibia. One of the reasons there may not be a big difference seen between single and double-bundle ACL reconstructions is that the distance between the two attachment sites is not that great, so placing a graft in the middle may not show a big difference.
16. Why is ACL reconstruction surgery done?
The ACL is important to prevent rotation of the tibia on the femur. In particular, anterolateral rotation, which can occur with twisting and pivoting activities, occurs after an ACL tear. In addition, the tibia tends to slip forward on the femur when one is ACL deficient. This particularly can be a problem for the posterior horn of the medial meniscus because it sees extra stress and can tear. ACL reconstructions that are performed in patients who note instability, but also in younger patients who may participate in twisting, turning, and pivoting sports to ensure that they do not tear their meniscus and develop osteoarthritis later in their lives.
17. What type of ACL reconstruction should be performed for a teenager?
In general, the International Olympic Committee statement notes that teenagers who tear their ACL should have an ACL reconstruction sooner rather than later to protect them against having both cartilage damage and meniscus tears. This can ultimately lead to development of osteoarthritis. One of the most important things to assess in the teenager is if their growth plates are still open or not. If the growth plates are still open, then placement of bone plugs or fixation hardware across the growth plates should be avoided to minimize the risk of a growth plate arrest. Usually, this means that these patients have ACL reconstructions with hamstring grafts. The problem with ACL reconstructions in teenagers is very problematic because we know that multiple studies have reported that the risk of an ACL tear in either the same knee or the opposite knee is roughly 30% before they end their teenage years. Thus, most physicians will ensure that teenagers pass a functional sports test prior to returning back to sport to minimize their risk of having an ACL graft re-tear.
18. When should ACL surgery be performed for a partial ACL tear?
A partial ACL tear can involve one of the bundles of the ACL alone. In particular, if the posterolateral bundle of the ACL tears and the patient notices difficulties with twisting, turning, and pivoting activities, then a single-bundle posterolateral bundle reconstruction of the ACL may be indicated. In these circumstances, if the anteromedial bundle is still pretty much intact, it would be recommended not to take it out and perform a complete reconstruction, but rather to perform a single bundle reconstruction to address the problems with twisting, turning, and pivoting.
19. When should an ACL reconstruction be performed with a quadriceps tendon autograft?
The use of a quadriceps tendon autograft for ACL reconstructions is a relatively new graft choice for many people. It is felt to possibly be a better option for some pediatric patients then utilizing the hamstring grafts because the graft volume may be larger. In terms of adults, there is not enough good science presently to decide whether the graft should be used with a bone plug or not, if there should be a full-thickness or partial-thickness graft, and if the rehabilitation protocols should be changed. A recent Danish National Registry study has reported that the use of quadriceps tendon autografts has a 4 to 5 times increased tear rate than either a patellar tendon autograft or a hamstring autograft. It does not appear that this was due to a learning curve or any other identifiable issue other than the fact that the graft was a quadriceps tendon graft. Therefore, some of our colleagues who were performing many quadriceps tendon grafts in Scandinavia have stopped using them for ACL reconstructions at the present time.
20. Why can’t I straighten my knee after an ACL reconstruction?
There can be many causes of difficulty with straightening one’s knee after an ACL reconstruction. These can include difficulty with rehabilitation after surgery where one does not regain full extension, having their ACL graft hypertrophy over time and causing a “cyclops lesion,” which can be a ball of tissue which can prevent full extension, or having technical issues with the ACL reconstruction graft whereby the graft is placed too anterior on the femur and one cannot straighten their knee. In general, the treatment for this initially is therapy, often using a dynamic extension splint to see if the patient can overcome their lack of full extension. If therapy does not work, then obtaining an MRI scan to look for a cyclops lesion may be indicated. In addition, surgical treatment can include debridement of a cyclops lesion, a notchplasty, or if it is a postoperative rehabilitation issue, an arthroscopic posterior capsular release may be indicated in some patients to help them regain full extension.
21. How long can I walk after an ACL reconstruction?
For those who have a first-time ACL reconstruction using a standard graft, patients are usually allowed to weightbear as soon as their surgical blocks wear off after surgery. In general, they can then proceed to weaning off of crutches when they can walk without a limp. We have found that most of our patients are able to wean off of crutches at about the 2-week point after surgery. However, some patients may take longer to wean off of crutches and should not use the timeframe exclusively, and should ensure that they are not limping before they completely discontinue the use of crutches.
22. What is an ACL reconstruction with an autograft?
An autograft is by far the best choice for almost all ACL reconstruction procedures. This is whereby one uses one’s own tissue rather than cadaver tissue. Cadaver ACL reconstruction grafts are best utilized in those who have had multiple ACL reconstructions whereby one’s own tissue is no longer available or in older patients who may be more sedentary and can afford the time to let a cadaver graft heal in biologically, which can take 9 to 12 months or more after surgery. In general, the definition of “older” patients varies among surgeons, whereby we feel that most patients up to the age of 60 can utilize their own tissue in most cases.
23. Is an ACL reconstruction procedure painful?
An ACL reconstruction procedure requires the harvesting of grafts, drilling of tunnels and bone, and often can have associated meniscus repairs with the procedure. Therefore, we expect most patients to require the use of pain medicines for a minimum of 2 to 7 days after surgery to address this. In general, starting physical therapy early and using ice after surgery can help one to decrease the perioperative pain degrees and can help one to minimize the use of narcotic medications.
24. When can one run after an ACL reconstruction?
The ability to run after an ACL reconstruction depends upon many factors. In particular, one has to know if it is a first time or revision ACL reconstruction and if there were any complex meniscus repairs associated with the ACL reconstruction. In these circumstances, one may need to put off running after surgery. In addition, if one has a significant amount of arthritis or knocked off a piece of cartilage and has a localized area of arthritis, returning back to impact activities may not always be indicated after an ACL reconstruction procedure. In our patients who have an ACL reconstruction, we would like them to have at least four months of physical therapy and to demonstrate that they can perform a single-leg squat with no valgus collapse prior to returning back to running. This usually occurs at between 4 and 5 months after surgery.
25. When can I return back to work after an ACL reconstruction procedure?
Returning back to work after an ACL reconstruction is a very individualized decision. In those people who have desk jobs, they can often return back to work for partial work days within 7 to 10 days, as long as they can ice and elevate their knee if there is any risk of swelling. For those patients who require the use of ladders, stairs, twisting or turning, or lifting patients, the time can vary from 4 to 7 months after surgery, depending upon the type of graft, associated other surgeries with the ACL reconstruction, and their ability to have their overall strength and endurance return.
26. When should one have an ACL reconstruction versus a repair?
Historically, ACL repairs were found to function poorly and therefore ACL reconstructions were developed. More recently, some academic centers have looked at ACL repairs in very select situations. These usually involve tears that are off the femur, that do not have any intrasubstance stretch, and that are treated in the “acute” situation, which can vary anywhere from days to just a few weeks. To date, the outcomes presented at scientific meetings is quite variable with a failure rate of anywhere from 20% to 80%. Therefore, one should be cautious about considering an ACL repair over reconstruction, and unless one is involved in a research study, it can be definitively said that the chances of having a better outcome currently are better using reconstructions instead of repairs.
27. When should a meniscus repair be performed with an ACL reconstruction?
It is best to perform meniscus repairs concurrently with the ACL reconstruction. This is because the ACL reconstruction will make the knee more stable and not put extra stress on a meniscus repair. In addition, it has been well documented that the drilling of tunnels associated with the ACL reconstruction can also release good growth factors into the knee, which will increase the chance of meniscus repair healing. While in the past there were some surgeons who performed a meniscus repair first and then came back to perform an ACL reconstruction, with today’s technology and tools, this is only done in patients who may have a staged surgery with bone grafting for an ACL reconstruction revision surgery and not for a first-time ACL reconstruction procedure.
28. What is the long-term prognosis for ACL reconstructions?
In general, a well-done ACL reconstruction can function quite well for 20 years or longer. This is some of the longest follow-up data that we have in scientific studies on ACL reconstruction grafts. The biggest risks for ACL reconstructions long term is in those patients who had their meniscus taken out rather than repaired. These patients are at a much higher risk for the development of osteoarthritis over the long term.
29. When should an ACL reconstruction be performed with stem cells?
Unfortunately, the use of stem cells is strictly regulated in the United States by the FDA. Therefore, one cannot have true “stem cell” surgery concurrent with an ACL reconstruction procedure unless one is involved in a strictly regulated FDA-approved study. The use of centrifuged bone marrow, most commonly obtained from the iliac crest, has been often used in the lay press to report as stem cells. However, the amount of stem cells in bone marrow aspirate concentrate is quite low, and I believe that other growth factors present may augment ACL reconstruction graft healing. However, there are no studies to date that have actually documented that any of these bone marrow aspirate concentrate (BMAC) augmentations of ACL reconstructions helps the grafts to heal faster, better, or change the natural history compared to a graft reconstruction performed without these injections.
30. What is an ACL reconstruction with an internal brace?
The use of an internal brace utilizes a surgical tape to try to augment an ACL reconstruction graft. To date, there are few studies that can determine whether this helps ACL reconstruction graft healing or not. Historically, the use of synthetic devices concurrent with ACL reconstruction grafts, such as the Ligament Augmentation Device by 3M, found there were no differences or any benefits in using this time of ACL reconstruction augmentation.
31. Why do I have shin pain after an ACL reconstruction?
Some patients can have shin pain after an ACL reconstruction because the surgical tunnel in the tibia has been drilled through the shin to place the graft in the joint. Other causes of shin pain after an ACL reconstruction can include hardware irritation or the development of a cyst around a bioabsorbable ACL fixation device.
32. Why do I have numbness after an ACL reconstruction procedure?
Almost all patients develop some numbness after an ACL reconstruction procedure. This is because the nerves from the saphenous nerve, especially the infrapatellar branch of the saphenous nerve, cross from the inside over the top to the outside of the knee. Patients with patellar tendon graft incisions and most hamstring incisions therefore will develop numbness over the front of their knee. In addition, patients who may have meniscus repairs to either the medial or lateral meniscus will also develop numbness to some extent around the surgical incisions.
33. What does “prehab” mean before an ACL reconstruction?
Some patients who tear their ACL will have a very stiff and swollen knee right after their injury. If they do not have a concurrent meniscus or other injury to their knee which requires surgery sooner rather than later, such as a radial tear of the meniscus, a bucket-handle tear of the meniscus, or a posterolateral corner injury, these patients are often sent for “prehab” to try to get their knee motion improved and try to get the swelling down in their knee prior to surgery. This is done because the risk of getting stiff after an ACL reconstruction can be increased if one has a stiff and swollen knee going into surgery. Therefore, having a good physical therapy program around the time of the ACL reconstruction is very important to ensure the best outcomes long term.
34. When should an ACL reconstruction be performed in patients over age 50?
Patients who are over age 50 who note difficulty with twisting, turning, and pivoting, especially those who ski or play court sports, should consider an ACL reconstruction as long as they do not have significant arthritis in their knee. If they have associated meniscus tears, it would also be recommended to repair these tears to both protect their ACL grafts and to minimize the risk of arthritis over time. In our series, we have found that the outcomes of patients that are older than age 50 are equal to those in the teenage and 20-year-old age range, so age by itself does not mean that someone should not undergo an ACL reconstruction procedure.
35. How can one interpret their x-rays after an ACL reconstruction procedure?
There are several peer-reviewed articles in the literature which note where ACL reconstruction tunnels should be optimally placed. In general, these are ranges of placement rather than saying a graft should be exactly in a position. In general, on a lateral knee x-ray, the ACL tunnel and hardware should not be above Blumensaat’s line. This would indicate that the graft is too anterior or central. In addition, placement of the ACL tibial reconstruction should be approximately 40% of the way from the front to the back of the tibia on the lateral x-ray.
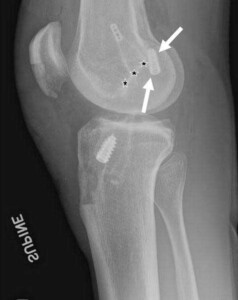
Lateral kneex-ray demonstrating anatomic positions of a revision ACL reconstruction tunnels. Note that the titanium fixation screw in the femur is located below Blumensaat’s line (denoted by stars) and in the posterior quadrant of the femur. In this position, the ACL reconstruction graft is best able to reproduce the normal function of the ACL. The original ACL tunnel denoted by the metal button was not placed anatomically and lead to ACL graft failure.
CLICK IMAGE TO ENLARGE
36. What are important recovery tips after ACL reconstruction surgery?
One of the most important recovery tips after an ACL reconstruction surgery is to ensure that one decreases the amount of swelling they have immediately after surgery so they can advance their rehabilitation protocol. One of the hardest things to do after ACL reconstruction is to regain full extension, so placing a pillow under one’s heel and letting gravity straighten out their knee can be an important part of the early rehabilitation program. Placing a pillow under one’s knee, while it may help one to feel better, often results in the knee having more blood leak into it and can make the hamstrings go into spasms, so it is difficult to straighten one’s knee out. In addition, as one advances in their rehabilitation program, taking baby steps forward to ensure that one does not have pain and swelling is important. Swelling often causes the muscles to atrophy, so avoiding swelling can ensure that one’s rehabilitation program advances in a timely fashion over the long term.
37. When are titanium screws used for ACL reconstruction surgeries?
Titanium screws are considered the gold standard for patellar tendon autograft reconstructions. In addition, they are considered the gold standard for most grafts that use a bone plug. Bioabsorbable fixation or other type of fixation, such as a cortical button fixation, are most commonly used for soft tissue reconstruction grafts. Titanium screws do not interfere with a future ACL reconstruction postoperative MRI and can be more easily visualized on x-rays to help determine one’s graft placement.
38. What causes knee popping after an ACL reconstruction?
Knee popping in the initial months after an ACL reconstruction can be very common. Most commonly, it is due to some swelling within the knee causing the overall knee viscosity to be decreased. Normal tissues can then having popping and cracking as one flexes and extends their knee. In general, most cases of popping go away with time as one’s quadriceps muscles get stronger and the swelling goes down. Nonpainful popping in general is due to normal tissues gliding, whereas painful popping needs an assessment by one’s surgeon to determine its cause.
39. Should one use ibuprofen after ACL reconstruction graft surgery?
In general, we discourage the use of anti-inflammatory medication such as ibuprofen or Naprosyn for the first 3 to 4 months after ACL reconstruction surgery. This is because these medications can interfere with bone healing and also with collagen cross-linking. If one needs a non-narcotic medication, the use of acetaminophen is usually recommended for most patients.
40. What are the symptoms of ACL reconstruction graft failures?
Patients who have ACL reconstruction graft failures may note difficulty with twisting, turning or pivoting. In addition, they may develop pain along the inside back part of their knee, which could indicate that they have an associated meniscus tear because of the knee being unstable. The most definitive way to determine if an ACL reconstruction graft is unstable is to have a physical exam and determine if one has a pivot shift test that is positive. In general, having a positive pivot shift test is associated with a stretched out or torn ACL reconstruction graft, and this test is more definitive than obtaining an MRI scan, whereby a loose ACL reconstruction graft may appear intact on the MRI scan.
41. What is the healing process for an ACL reconstruction?
The healing process for an ACL reconstruction graft can depend upon the type of graft. In general, patellar tendon grafts heal into the bone tunnels at 6 weeks. Hamstring tendon grafts may take up to 3 months to heal in the tunnels, whereas cadaver grafts can take 3 months or longer. In terms of the main graft substance healing that is within the joint, it is generally at its weakest point between 3 and 4 months after surgery, and having a good blood supply restored to the tissue can take 9 to 12 months or longer. A lot of research has gone into studying this and there are no definitive answers for individual patients at the present time.
42. Is an ACL reconstruction performed as a day surgery?
The vast majority of ACL reconstruction procedures nowadays are performed as a day surgery. However, if there are other ligaments concurrently reconstructed, or complex meniscus repairs, the patients may need to stay overnight in a 23-hour stay unit and be discharged the next morning if there are any concerns about the ability to control their pain.
43. What type of anesthesia can be used for ACL reconstructions?
In general, the decision about what type of anesthesia one has for their ACL reconstruction should be made with an anesthesiologist. As orthopaedic surgeons, we can usually work with an epidural, spinal, or some type of general anesthesia. It is difficult to perform ACL reconstruction grafts under local anesthesia, because the assessment of meniscus tears and the positions that the knee has to be bent into can be compromised if the patient is guarding. It may not allow for all pathologies to be diagnosed and treated appropriately.
44. When should one use crutches after an ACL reconstruction?
For ACL reconstructions that do not require one to be on crutches for an extended period of time due to other concurrent surgeries, the general belief is that one should stay on crutches until they can walk without a limp. In general, this usually occurs around the 2-week timeframe for most patients.
45. When is one allowed to go back to full activities after an ACL reconstruction?
The return to sports and other activities after an ACL reconstruction is generally not time dependent, but we do know that the 9-month timeframe seems to be a time whereby athletes who go back prior to this time have a higher risk of having their graft re-tear. An assessment of whether one uses their own tissue or a cadaver graft, or if one has other ligament reconstructions or meniscus tears, must also be taken into consideration. It is especially important in teenagers to ensure that they have a full return of strength, endurance, agility, and balance prior to returning back to sports because their risk of re-tear can be much higher if they do not pass some type of functional sports assessment. In addition, returning back to sports prior to 9 months with a cadaver graft is generally not indicated because of a higher risk of re-tear.
46. What are some ACL reconstruction questions to ask one’s surgeon?
There are many questions that one could ask to ensure that they comprehend their ACL reconstruction procedure. First, it is important to determine if the surgeon is going to use their own tissue with an autograft or if they will use a cadaver tissue with an allograft. This can sometimes be the most important factor in determining the success rate of an ACL reconstruction. One can also ask about what type of autograft, which could be a patellar tendon, hamstring, or quadriceps tendon. All of these types of autografts can have specific uses for which they are most beneficial for a patient.
47. Can one have an ACL reconstruction in a varus knee?
Having a varus knee by itself does not necessarily contribute to extra force on ACL reconstruction graft. However, if a patient has a varus thrust where they put extra stress on the outside of their knee, this can lead to overload of an ACL reconstruction graft, which can cause it to either stretch out or tear over time. Most patients who have a varus thrust gait may have some arthritis of the inside of their knee which causes some thrusting or they may have a tear of their lateral collateral ligament on the outside of their knee which can lead to overload of an ACL reconstruction graft.
48. When can one golf after an ACL reconstruction?
In general, we want patients to have a good restoration of strength and stability prior to returning back to golfing. In most circumstances, with a first-time ACL reconstruction and no other specific things going on in the knee, one can initiate golf at about 4 months after an ACL reconstruction procedure.
49. When should one consider an ACL reconstruction versus stem cell therapy?
Due to FDA regulations, true stem cell therapy is not available in the U.S. Therefore, the use of bone marrow aspirate concentrate, commonly called “stem cells” in the lay press, essentially has minimal to no chance of causing a completely torn ACL to heal. Therefore, most patients who have a complete ACL tear should consider a reconstruction to treat their problem if there are problems with twisting, pivoting, and other activities.
50. When should one have an ACL reconstruction versus an osteotomy?
In some patients that have arthritis of the inside part of their knee and who are bowlegged, it may be difficult to determine if their problems are coming from their ACL tear, causing instability, or from their bowleggedness and arthritis on the inside part of their knee causing pain. Therefore, it is important to screen these patients, often with a medial unloader brace, to see if their pain goes away and they can function better by unloading the compartment. In this circumstance, the use of a proximal tibial osteotomy to unload the medial compartment and shift the alignment into neutral rather than being bowlegged may be beneficial. In patients that may have some arthritis on the inside part of their knee, but they truly have instability, the use of an ACL reconstruction in these patients over an osteotomy may be indicated.
51. When is bone grafting used for an ACL reconstruction?
Bone grafting for an ACL reconstruction is almost always utilized for a patient that has had a previous failed ACL reconstruction graft. In some of these circumstances, the previous tunnel may become enlarged from the type of graft to the point where one cannot proceed with a revision reconstruction with a new graft without having a high likelihood of having the new graft fail because of a very large tunnel. In these circumstances we would clean out the tunnel arthroscopically and place in bone graft to fill in the tunnels. Once the bone graft heals, one could then proceed with a revision ACL reconstruction and place the new tunnels in a correct anatomic position.
52. When can an ACL reconstruction be performed in those over age 60?
There is no upper age limit to an ACL reconstruction because it is mainly dependent upon the patient’s activity levels, other medical problems, and if they have instability. For those older patients, we will commonly place them into ACL braces to see if that will be sufficient to restore their stability and function. In some circumstances, the braces may work, but when the patients do not have the braces on they have significant problems with twisting, turning, and pivoting. In those circumstances, it may be indicated to proceed with an ACL reconstruction. It is important to screen these patients to ensure that they have gone through proper rehabilitation and consider the use of an ACL brace to see if they would benefit from a surgery prior to proceeding directly to an ACL reconstruction for the torn ACL.
53. When is an ACL reconstruction using an iliotibial band used?
Most ACL reconstructions using an iliotibial band are used in very young patients with open growth plates. In these circumstances, it is important to avoid the growth plates to ensure that growth plate arrest and angular deformities of the knee do not occur. Historically, several decades ago, the ACL was often reconstructed with an iliotibial band. Today, this is mainly utilized in patients with wide open growth plates, commonly in the age 5-10 age group.
54. What is the operation time for an ACL reconstruction?
The operation time for an ACL reconstruction can be dependent on many factors. If it is just the ACL reconstruction itself and there are no other meniscus tears or other ligament injuries that are being reconstructed, the process involves harvesting and preparation of the graft, drilling the tunnels in the proper positions, and then passing and fixing the graft in the tunnels. It is also important to recognize that the whole knee must be checked to ensure that there are no other injuries present because missing an injury, such as a lateral meniscus root tear, can result in an ACL reconstruction graft failing. In general, we recommend the use of one’s own tissue rather than cadaver tissue for ACL reconstructions. The use of cadaver tissue would also cut down the operative time because one does not have to harvest the graft from the operative knee, but over time, the failure rate of allografts is much higher than using one’s own tissue.
In general, a well-done and efficient ACL reconstruction can take anywhere from 25 minutes to an hour. If one has assistants present, the operative time can commonly be decreased. In addition, high-volume surgeons often have a team that knows the steps in advance, so the operative time can commonly be decreased in these cases.