If you are experiencing pain behind the knee, it could be a PCL tear or strain.
What is the PCL (Posterior Cruciate Ligament)?
The ligament located on the back and middle of the knee is known as the posterior cruciate ligament, or the PCL. It is one of several ligaments that connect the femur (thighbone) to the tibia (shinbone). The posterior cruciate ligament is the strongest ligament of the knee and thus, it is injured less often accounting for about 3-37% of all knee injuries.
PCL Tear Symptoms
Posterior cruciate ligament tears can cause:
- Problems decelerating
- Problems going down stairs and inclines
- Problems twisting, turning, or pivoting
- Pain over the anterior aspect of the knee
A posterior cruciate ligament injury is often caused by a powerful force—in many cases from sports trauma. PCL injury causes might include a bent knee hitting something very hard (for example, a dashboard in a car accident or a hockey player hitting the goalpost) or a football player falling on a knee while it is in the bent position.
PCL Diagnosis
Dr. LaPrade will assess signs of a torn PCL with a detailed clinical exam, x-rays, kneeling posterior knee stress x-rays, and almost always, an MRI scan to determine the extent of the injury and concurrent injuries to determine the recommended course of posterior cruciate ligament tear treatments. In general, many isolated PCL injury will heal over time; it is important to diagnose this particular ligament tear early to attempt to get them to heal in a stable position rather than in an elongated and nonfunctional position. While the results of an MRI scan are helpful for an acute injury evaluation, they are not very useful in the case of a chronic injury to evaluate for a PCL tear because they can show an intact posterior cruciate ligament, which may be unstable because it has healed in an elongated position. In this case, stress x-rays are required to diagnose the extent of the tear.
PCL Injury Test
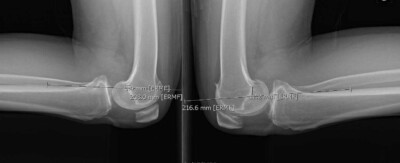
The diagnosis of a torn posterior cruciate ligament depends upon assessment of the patient’s posterior knee translation. PCL injury test involves examining the patient from the side to see if there is any posterior step off, performing a quadriceps active test and also performing the posterior drawer test in neutral rotation. In addition, a patient should have bilateral posterior knee stress radiographs to objectively determine the amount of increased posterior translation on the injured knee.
Posterior Cruciate Ligament Pain Grading
Posterior cruciate ligament pain injuries are classified according to the amount of injury to the functional ligament:
- Grade 1 PCL Sprain: A small partial tear
- Grade 2 PCL Sprain: A near complete tear
- Grade 3 PCL Tear: A complete tear whereas the ligament becomes non-functional; usually this occurs with injuries to other knee ligaments (most commonly the posterolateral knee structures)
Most isolated grade 1 and 2 PCL sprain injuries should be treated with a non-operative program to include functional rehabilitation of the quadriceps mechanism and the possible use of a jack brace to help reduce the knee into a normal (neutral) position. Dr. LaPrade strongly encourages patients with a partial PCL tear to participate in this rehabilitation program.
Are you experiencing pain in the ligament behind your knee or suspect a torn ligament behind your knee? You could have a PCL strain or tear.
There are two ways to initiate a consultation with Dr. LaPrade:
You can provide current X-rays and/or MRIs for a clinical case review with Dr. LaPrade.
You can schedule an office consultation with Dr. LaPrade.
(Please keep reading below for more information on this condition.)
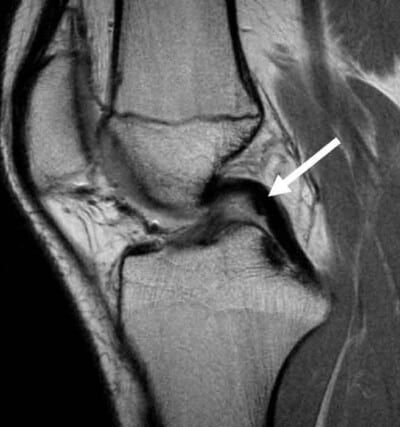
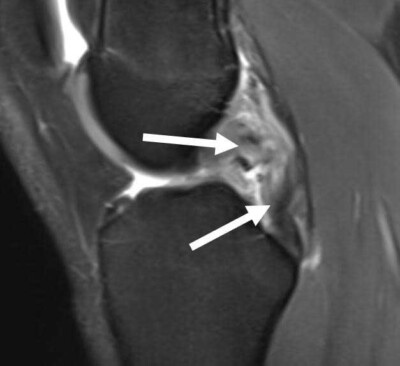
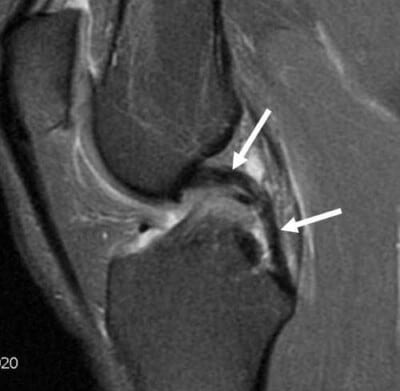
How to Read a PCL Tear MRI
PCL Tear Treatment
Patients who have a complete PCL tear with less than 8 mm of posterior translation can be considered for a non-operative rehabilitation program in special circumstances. However, in most patients who have 8 mm or more of increased posterior knee translation, there is a much higher likelihood than not that these patients will need a posterior cruciate ligament reconstruction surgery to improve their knee function and decrease their chances of developing knee arthritis. Thus, in a higher-level athlete, it is usually recommended to proceed with the PCL knee reconstruction because results of acute reconstructions are much better than chronic reconstructions.
When Dr. LaPrade makes the determination that a patient does need a PCL reconstruction, he thoroughly assesses the patient to see if there is any concurrent injury. Approximately 90% of patients who have persistent PCL tear symptoms limiting their function also have a posterolateral corner, posteromedial injury or other associated injury. Thus, the incidence of isolated PCL reconstructions in our own series is approximately 10% of the total posterior cruciate ligament reconstructions performed.
Dr. LaPrade’s surgical rehabilitation technique for a PCL reconstruction is an endoscopic-based double bundle reconstruction with allografts using a technique that he has developed. It utilizes minimal incisions and does not violate the quadriceps mechanism like conventional posterior cruciate ligament reconstruction surgery techniques. The double bundle PCL reconstruction has been extremely effective in restoring knee stability back to the patient both objectively with PCL stress x-rays and subjectively based on patients independently evaluating their outcome scores.
PCL Surgery Recovery
PCL surgery recovery involves patients to initiate prone knee flexion at 0-90° on day one. They use a PCL jack brace for six months postoperatively to reduce the posterior gravitational stress to the knee. Patients initiate a partial protective weight-bearing program at six weeks postoperatively and wean off of crutches at that point when they can walk without a limp. Patients may initiate the use of a stationary bike and leg presses to a maximum of 70° of knee flexion at 6 weeks postoperatively.
We have found that our PCL rehab protocol, which may be considered aggressive by other treatment centers because we initiate motion with PCL reconstructions on postoperative day one , has not resulted in any of our grafts stretching out over time and has demonstrated a much quicker return of knee motion, decreased risk of knee stiffness and high level function.
Related Studies
PCL Injury FAQ
If you are experiencing pain behind the knee, it could be a PCL tear or strain.
1. What is the PCL (Posterior Cruciate Ligament)?
The ligament located on the back and middle of the knee is known as the posterior cruciate ligament, or the PCL. It is one of several ligaments that connect the femur (thighbone) to the tibia (shinbone). The posterior cruciate ligament is the strongest ligament of the knee and thus, it is injured less often accounting for about 3-37% of all knee injuries.
2. What is the PCL in the knee?
The PCL, or posterior cruciate ligament, is the strongest ligament in the whole knee. It sits in the center and back of the knee and prevents the knee from slipping backwards. It is most important for function on a bent knee, usually when the knee is bent to about 90 degrees.
3. What is a PCL injury?
A PCL injury occurs when the main ligament in the back of the knee, the PCL, is torn. This most commonly occurs when somebody either hyperextends their knee or hits their knee against something when their knee is bent. This can be a dashboard injury in a motor vehicle accident, or it can be an athlete that falls down while playing a sport onto a bent knee.
4. What does a PCL tear feel like?
Most athletes who tear their PCL describe a tearing sensation within their knee. Most do not describe a “pop” which is commonly a bone bruise which happens with an ACL tear. A PCL tear commonly causes just a little bit of swelling in the knee, and when it occurs by itself (that is without any other ligaments torn), there may not be a lot of swelling within the knee.
5. What is a PCL tear in the knee?
A PCL tear in the knee is when the major ligament of the back of the knee is torn. This most commonly happens when an athlete has a hyperextension injury or falls on a bent knee against a hard surface. In motor vehicle accidents, this may occur when a passenger hits their knee against a dashboard.
6. Where is your PCL? Where is the PCL located?
The PCL is located in the back of the knee. Hence, “posterior” means the back of the knee. It is the main ligament that prevents the knee from slipping backwards, or posteriorly. It is within the knee joint itself and can be seen arthroscopically, adjacent to the anterior cruciate ligament (ACL).
7. Where is PCL pain?
PCL pain has been described as deep within the knee and dull. There is not usually a sharp pain described with an isolated PCL tear. In some circumstances, such as with football lineman, the dull ache can be difficult to determine from wear and tear from normal sports activity contact and the PCL tear may go unrecognized for a few days.