Why did my ACL Reconstruction Surgery Fail?
An ACL reconstruction is one of the most common surgical procedures in orthopaedic surgey. Although only 10% of grafts fail, this is still a large number of cases. There can be many reasons for an ACL reconstruction failure.
The most common reason for an ACL graft to fail is due to technical issues with the original surgery. An ACL reconstruction is very technical and it is well recognized that surgeons who perform more of these procedures have improved outcomes. However, the majority of ACL reconstructions performed in the United States are performed by surgeons who perform ten (10) or less each year. For that reason, misplaced graft reconstruction tunnels are still a very common cause of an ACL reconstruction failure. This can be due to placement being too posterior on the tibia, which results in a central graft that does not control rotation, or too anterior placement on the femur, which can result in the graft stretching out as knee flexion returns.
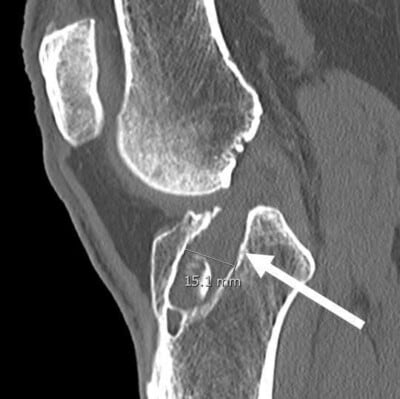
CT scan of a failed ACL reconstruction demonstrating the wide diameter of the previous ACL tibial reconstruction tunnel. In some patients, these tunnels will become larger than when they were originally reamed, especially for hamstring autografts or cadaver allografts. If they are larger than 12 to 14 mm in diameter, or are in a position where an anatomic positioning of the ACL reconstruction graft would break into the previously malpositioned tunnel, then a two-staged surgery would be recommended. This would involve bone grafting of the tunnels and, once the tunnels heal in approximately four to six months, to proceed with a revision ACL reconstruction in the correct anatomic position.
CLICK IMAGE TO ENLARGE
The second most common cause of ACL reconstruction failure is due to untreated secondary instabilities. This could include a posterolateral corner injury, a meniscal root detachment, or a lack of the posterior horn of the medial meniscus. It is well recognized that a deficiency of these areas, and other areas to include an unrecognized PCL injury, medial knee injury, alignment issues in patients who have arthritis and other issues, are also common causes of ACL reconstruction failures. For this reason, the work-up for an ACL revision surgery must include evaluation of the secondary restraints of the knee and the integrity of the posterior horn of the medial meniscus.
Traumatic reinjuries also can occur, but in general are not felt to be the most common cause of ACL graft failure. In this circumstance, an athlete sustains a reinjury to their knee with the ACL graft being torn. While less common, athletes in this circumstance may have improved overall outcomes with an ACL revision surgery
Another important issue to evaluate for ACL reconstruction graft failures from ACL knee surgery is biologic issues. Literature has reported that patients who are less than 25 years of age have a much higher risk of ACL graft failure with an allograft reconstruction. In addition, a small number of patients may have their own grafts not completely heal and tear over time. Reasons for early allograft failure could include an immune response and lack of graft incorporation, a too early return back to high level activities prior to graft incorporation or issues with the graft itself to include unrecognized tearing within the graft or use of irradiation to sterilize the graft (which has been shown to increase the risk of graft failure).
Has your ACL reconstruction surgery failed? You may be a candidate for an ACL Revision Reconstruction.
There are two ways to initiate a consultation with Dr. LaPrade:
You can provide current X-rays and/or MRIs for a clinical case review with Dr. LaPrade.
You can schedule an office consultation with Dr. LaPrade.
(Please keep reading below for more information on this treatment.)
How to Perform ACL Revision Surgery
Thus, the work-up for ACL revision surgery has to include an evaluation of biology, evaluation of the patients alignment and their secondary restraints, a careful assessment of the posterior horn of the medial meniscus and also an evaluation of the previous reconstruction tunnel placement and size. Soft tissue ACL reconstruction grafts often cause graft reconstruction tunnel enlargement over time and a careful assessment for this must be performed.
When all factors have been evaluated, an assessment can then be made if a one stage or two stage reconstructions are necessary. There are certain times when trying to perform a one stage ACL reconstruction may significantly increase the risk of failure of the revision graft. Possible treatment scenarios include patients undergoing an autograft or allograft revision reconstruction, either as a first stage or as a second stage surgery after bone grafting the tunnels first and/or a combined proximal tibial osteotomy. Concurrent procedures with the revision ACL reconstruction could include meniscal repairs, meniscal transplants, posterolateral corner or medial knee reconstructions.
It is very rare that the evaluation of a failed ACL reconstruction graft is easy. There is usually a reason why the graft failed and a very careful assessment must be performed including long leg alignment x-rays, possible varus/valgus stress x-rays, a Rosenberg view to look at joint space narrowing and an MRI scan to look at the location, size and position of the previous ACL reconstruction graft tunnels as well as the status of the meniscus and articular cartilage of the joint.
A very thorough physical exam is necessary but these secondary studies are often required to choose the best plan of treatment for a revision ACL reconstruction. In general, the success rates in the literature for ACL revision surgery are approximately 75%. A very careful assessment of the cause of the graft failure is necessary to try to maximize an individual patient’s outcome with an ACL revision surgery.
Post-Operative Protocol for Revision ACL Surgery
The rehabilitation program for a revision ACL surgery needs to progress slower than those for a primary (first time) ACL reconstruction. In most patients, we keep them on crutches but with full weight bearing to minimize stress on the ACL graft. The timing of advancement of the specific rehabilitation exercises is generally slowed down by about 50% and a return to full activities is rarely allowed prior to 9 months after surgery.
Related Studies
- Biomechanical Comparsion of Anatomical Single and Double Bundle ACL Reconstruction
- Femoral Cortical Suspension Devices for Soft Tissue ACL Reconstruction
- Biomech Comparison of Tibial Fixation for Soft Tissue ACL Grafts on the Tibia
- Functional ACL Bracing – Current State
- Effects of Grade III PLC Injuries on ACL Grafts
Revision ACL Reconstruction FAQ
1. What is ACL revision surgery?
ACL revision surgery is performed when a first-time ACL repair or ACL reconstruction did not work and the surgery has to be redone. Usually, this requires an extensive workup because the results of ACL revisions are nowhere near as successful as the first time around. This usually requires alignment x-rays, lateral knee x-rays to the look at the tibial slope, an MRI to determine the meniscus volume (which can affect the ability of an ACL graft to heal), the presence of meniscal ramp tears or meniscal root tears, and also a combined physical exam and possibly varus or valgus stress x-rays if there is an unrecognized or untreated MCL or posterolateral corner (which includes an LCL (FCL) tear) injury present. In addition, most ACL revisions require a CT scan to look at the placement of the tunnels from the previous ACL reconstruction and to determine the size of the tunnels to determine if a bone graft may be necessary as a first stage surgery to fill in the tunnels when the tunnel is too large to place an ACL graft in for a first stage revision ACL reconstruction.
2. When ACL surgery fails?
The most common cause of ACL failure is a technical error in the first surgery. The two most common technical errors are placing the ACL reconstruction graft on the femur too anterior (away from the back wall) or placing the tibial tunnel too posterior (posterior to the anterior horn of the lateral meniscus). In almost every published study, these are the most common causes of an ACL graft failure. Other causes of ACL graft failures include a lack of a medial meniscus, because the medial meniscus is an important stabilizer to preventing the knee from slipping forward in an ACL deficient knee. When there is no medial meniscus, an ACL graft would be at risk for stretching out. Meniscal root tears can also cause an ACL graft to stretch out, and missed, or unrecognized, posterolateral corner or medial collateral ligament (MCL) tears can also cause an ACL graft to stretch out. In addition, patients who have an increased posterior tibial slope are at risk for having ACL grafts stretch out.
3. Can ACL surgery fail?
ACL surgery can fail, even in the best of circumstances. It is generally felt that a well-done ACL reconstruction has about a 5% chance of failure due to trauma. The most common cause of an ACL graft failure is a technical error with malposition of the original ACL reconstruction tunnels. Other causes of ACL failure include missed or unrecognized concurrent diagnoses, such as meniscal root tears, meniscal ramp tears, posterolateral corner injuries or MCL tears, or the original graft choice.
A large number of studies have indicated that the use of cadaver grafts (allografts) in younger patients have a much higher risk of failure. Thus, most ACL high-volume surgeons would use a patient’s own tissue for their ACL reconstruction when they are younger. In addition, patients who have a lot of laxity, especially patients who have increased heel heights or knee hyperextension, have a much higher risk of having cadaver graft or one’s own hamstrings graft stretch out, and these patients may be indicated for using a patellar tendon autograft. Failure of an ACL reconstruction needs a complete workup to ensure that the same problem is not repeated the second time around and to make sure that the patient has the best chance of success after a revision surgery.
4. When ACL surgery goes wrong?
As with any procedure, there can be technical issues with an ACL reconstruction which can make things more complicated. First, probably the most important thing is to ensure that all injuries that occur with an ACL are concurrently treated to provide the best chance of the ACL graft healing without having it stretch out and become loose. Issues that can occur with an ACL reconstruction surgery include fractures of the lateral femoral condyle, for which we have published peer-reviewed case reports on, breaking out the back wall, or soft bone which hinders fixation. Breaking out the back wall occurs on occasion when the bone is soft, and can be easily addressed by adding an extra incision and tying the sutures over a screw and washer. This should not slow down the rehabilitation program. In addition, when there is poor graft fixation due to soft bone, which is usually on the tibia, a screw and washer back up can be added to give the best chance of having the ACL graft heal.
5. How to know if ACL injury failed?
The best means to determine if an ACL reconstruction graft is torn is by either the patient’s history or by a good clinical exam. Unfortunately, MRI scans are not very effective for determining the function of an ACL graft. Usually, a patient will describe difficulty with twisting, turning, and pivoting and this usually indicates that an ACL reconstruction graft has failed, even if the MRI shows a stout ACL reconstruction graft present in the knee. In addition, the presence of an increased amount of anterior tibial translation on the Lachman’s test, usually a grade 2 Lachman’s test, as well as the presence of a pivot shift test of at least a grade 2, indicates that an ACL graft is nonfunctional and stretched out and probably not working sufficiently to prevent reinjury to the athlete. Other secondary signs of an ACL graft not working include bone bruises in the lateral compartment on an MRI scan (bone bruises on the posterior aspect of the tibia and the anterior aspect of the lateral femoral condyle). Less commonly, ACL stress x-rays or the use of a KT-1000 stress machine can also be used to objectively determine the increase in anterior tibial translation. It is felt that a 3 mm increase in anterior tibial translation compared to the contralateral knee is indicative of a nonfunctional ACL reconstruction graft.
6. What causes ACL reconstruction failure?
ACL reconstruction failure can be caused by many factors. First, if an athlete returns to competition prior to having full endurance, proprioception, strength and agility, they are at risk for an ACL reconstruction failure even if the graft is perfectly placed. Thus, a proper rehabilitation program and passing a sports specific functional test like the Vail Sports Test would be indicated for high-level athletes.
Similarly, going back to activities too soon after an allograft ACL reconstruction also puts one at risk for failure. This is because allografts can take up to 50% longer to heal compared to using one’s own tissue. This is believed to be the main reason why allografts fail up to 45-50% of the time in patients that are less than 25 years of age. Other causes of ACL reconstruction failure include technical errors with placing the tunnels in the wrong positions, meniscus root or ramp tears, posterolateral corner injuries, MCL injuries, and an increase in posterior tibial slope.
7. How to tell if your ACL graft failed?
Patients who have intact, but nonfunctional, ACL reconstruction grafts usually experience difficulty with twisting, turning, and pivoting. Sometimes these grafts may even look “normal” on an MRI scan. Patients may have swelling with activities also. Some athletes may also tear the posterior horn of the medial meniscus because of the fact that the medial meniscus is the next structure which prevents the knee from slipping forward when the ACL is nonfunctional.
In acute injury situations, there may be pain and swelling in the knee, although most patients feel that their ACL graft tears did not have as much pain and swelling as the original ACL did. This probably because the blood supply is not as well established in ACL grafts as it is from the middle genicular artery in one’s own ACL.
8. Stretched ACL graft symptoms?
It is important to recognize that a “stretched ACL graft” is probably equivalent to having no ACL graft. Thus, the patients would experience the same problems as those who have a lack of an ACL. This would include difficulty with twisting, turning, pivoting, deceleration, and participating in sports such as soccer, basketball, racquetball, football, and baseball. This would also include volleyball and gymnastics where one has to twist, turn, or pivot. Athletes who have difficulty with these activities should be evaluated carefully as to whether their ACL graft is nonfunctional.
9. ACL graft failure rate?
In general, the ACL graft failure rate depends upon a patient’s age and the type of graft. In general, the rate of failure for a patellar tendon autograft (from one’s own tissues) is lower than a hamstrings autograft. In addition, failure rates for allograft (from cadaver tissue) are higher than those for using one’s own tissue. Other factors include whether an athlete is hypermobile, where a patellar tendon graft has higher success rates, and the age of the patient/athlete. Younger patients, especially athletes in their teenage years, have much higher rates of failure (up to 30%), compared to patients in their 40s and 50s who may have failure rates of 2-5%. The ACL graft failure rate can also be affected by whether there are any cartilage or meniscus tears or other ligament injuries concurrent with the ACL injury.
10. ACL revision surgery recovery time?
It is currently believed that a revision ACL surgery recovery time should require at least a 50% longer rehabilitation program than a first time ACL reconstruction surgery. This is because the blood supply is not as good in a revision reamed tunnel as the first time around and biology seems to greatly affect ACL graft healing. In general, most revision ACL reconstructions take 9-12 months to adequately heal and for the athlete to recover their strength, endurance, proprioception and balance. Some level 4 studies have indicated that the use of biologics such as PRP may potentially increase the rate of healing for ACL revisions, but no good high-level studies have been able to confirm this as of yet.
11. Signs of ACL graft failure?
The signs of ACL graft failure can include swelling, pain within the knee, locking within the knee, a mechanical block (which can be due to a bucket-handle tear of the meniscus), lack of full motion, and difficulty with twisting, turning, and pivoting.
12. Revision ACL reconstruction rehabilitation protocol?
It is currently believed that biology needs to be respected more for revision ACL reconstructions than primary ACL reconstructions. Thus, the timeframe for advancement of activities is slower for revision ACL reconstruction to maximize the patient’s chance of success. In our practice, we have patients fully weightbearing after surgery, but they are on crutches a minimum of 4 weeks to ensure that they are unloading their ACL reconstruction graft initially. They wear an ACL brace through 6 months postoperatively to ensure that they do not have extra forces on their ACL when they twist, turn, or pivot. If they do not have any significant arthritis (cartilage problems), or complex other injuries, such as meniscus root repairs, LCL (FCL) reconstructions or MCL reconstructions, they may initiate a return to jogging program after the 4-month period and when they can perform a single-leg squat with no valgus collapse. Assessment of valgus collapse in the ACL reconstruction patients appears to be a very important way to ensure that patients have adequate strength before they start a jogging program. If they initiate a jogging program too soon, they may be damaging their cartilage because they may not have as good absorption and they also may be putting extra stress on their ACL reconstruction graft which could cause it to stretch out over time.
13. Revision ACL bone grafting?
It is very common for a patient to require a bone grafting procedure for a revision ACL reconstruction. Most surgeons who perform ACL revision surgery obtain CT scans of the patient’s knee to assess the original ACL reconstruction tunnel location and size. Tunnels that are larger than 12 mm, or which are malpositioned such that a correctly positioned tunnel would break into the malpositioned tunnel (or overlap with it), need to be bone grafted first. In our published series, we have found that we have significant reduced the rate of ACL reconstruction graft failure to 6% at 3 years postoperatively when bone grafting was performed in properly indicated patients, which is significantly less than a historical percentage of a 30% failure rate of ACL revision reconstructions. Thus, consideration for bone grafting when the tunnels are too large or when the tunnels would overlap with a properly placed tunnels for a revision ACL reconstruction should be considered in all patients.
14. ACL revision recovery
Because of the fact that ACL revision reconstructions require new tunnels, commonly concurrent with or overlapping with old tunnels, the blood supply in the bone to the ACL graft is not as good. Thus, one has to use caution to ensure that there is sufficient ability for the ACL graft to heal. Thus, ACL revision rehabilitation programs tend to be more conservative and advance slower to give the best chance for the ACL graft to heal. We initiate weightbearing immediately postoperatively but keep patients on crutches for 4 weeks. We also keep them in an ACL brace to protect their knee against any undue forces with twisting, turning or pivoting until at least the 6-month point. Patients that do not have arthritis and can perform a single-leg squat with no valgus collapse may be considered for initiation of a jogging or running program starting at 4 months postoperatively. However, it is important to ensure that the patients have adequate strength, balance, endurance, and agility prior to returning back to activities so they do not reinjure their ACL reconstruction graft. It is generally felt that a minimum of 9 months postoperatively is required for most ACL revision reconstructions to minimize the risk of a graft retear.