The meniscus is an important shock absorber of the joint. As one ages, the meniscus can become more brittle and is much easier to tear. An arthroscopic meniscectomy is performed in over 200,000 – 300,000 patients each year in the United States.
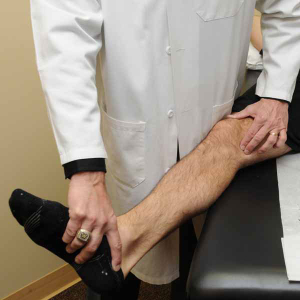
The current standard used to assess for the presence of meniscal tears is to palpate along the joint line while applying a varus or valgus stress to the knee. It is important to feel for associated crepitation within the joint when performing this and also check if the patient has any pain with this maneuver. If there is deep joint line pain with crepitation which reproduces the symptoms, the diagnosis is an underlying meniscus tear or articular cartilage injury until proven otherwise.
Another important test to assess for a meniscal tear is to have a patient maximally flex their knee or to have them perform a deep squat. In patients who have pain over the posterior aspect of the knee with these maneuvers, this is also considered a meniscus tear until proven otherwise. Other potential diagnoses include knee swelling or the possibility of a Baker’s cyst in the posterior aspect of the knee.
Standing radiographs should be obtained in all patients to determine if there is any joint line narrowing or osteophytes which could be indicative of some underlying osteoarthritis. In patients who have extensive joint space narrowing, we generally feel that an MRI is not indicated and would recommend that other means of treatment be performed to determine the etiology of the patient’s pain.